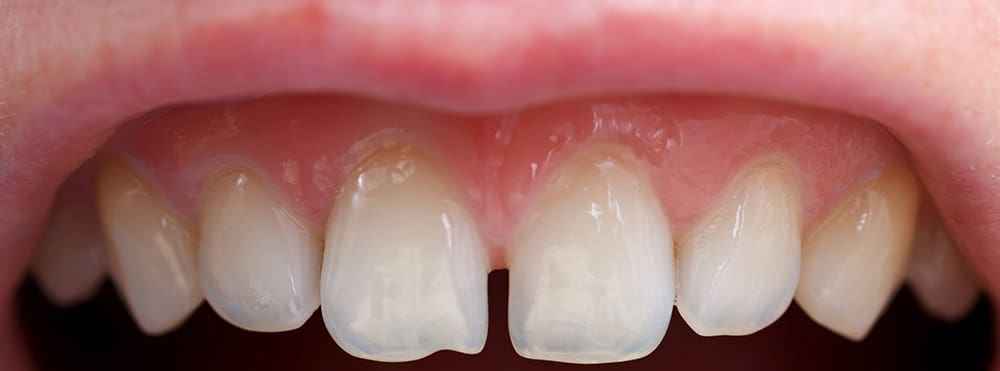
Tooth transparency is a phenomenon that often catches people off guard. It refers to areas of the tooth where light passes through more easily, giving a slightly translucent or glassy appearance. While some transparency is natural, excessive or uneven translucence can signal underlying enamel changes or structural issues. Understanding tooth transparency helps individuals recognize subtle changes early, prompting careful observation and potential corrective strategies.

Understanding Tooth Transparency
Tooth transparency occurs primarily due to variations in enamel density and thickness. Enamel, the hardest substance in the human body, is semi-translucent by nature. When enamel wears down or loses mineral content, light penetrates differently, creating visible translucent zones. Factors such as diet, acid exposure, and even genetics influence how noticeable these areas become.
Interestingly, transparency is not always uniform. Some teeth might show subtle translucence at the edges, while others display patches along the biting surface. Recognizing these patterns can provide insight into enamel health and guide further assessment.
Enamel microstructure plays a crucial role in this visual phenomenon. Studies indicate that variations in enamel rod orientation and inter-prismatic spacing can alter how light interacts with the tooth. These microscopic changes, though invisible to the naked eye, contribute to the perception of tooth transparency.
Common Causes Behind Tooth Transparency
The causes of tooth transparency are multifactorial. Acidic foods, excessive brushing, and enamel erosion are frequent contributors. Over time, these factors reduce enamel thickness, exposing the inner dentin and creating that translucent effect.
Genetics also plays a part. Some individuals naturally have thinner enamel, making their teeth more prone to transparency even without significant wear or external influence. Similarly, developmental anomalies can leave teeth more vulnerable to light penetration.
Lifestyle choices can intensify this condition. High consumption of citrus fruits, sodas, or acidic beverages accelerates enamel wear. Environmental factors, including fluoride levels in drinking water, can further influence enamel robustness and tooth transparency manifestation.
Detecting Tooth Transparency at Home
Detecting tooth transparency early is possible without advanced equipment. Simple visual checks in natural daylight can reveal unusual translucence along the edges or surfaces of teeth. Using a mirror, tilt your teeth at different angles to observe how light passes through.
Additionally, subtle texture changes may accompany transparency. Slight roughness or minor ridges often correlate with areas where enamel is thinning. This tactile approach, combined with visual inspection, allows for a comprehensive understanding of the tooth’s surface.
Digital photography can assist in monitoring changes over time. Taking consistent photos under similar lighting conditions can reveal incremental transparency that might not be apparent day to day. Tracking these shifts helps determine whether treatment intervention is warranted.
Treatment Method 1 – Remineralization Techniques
Remineralization focuses on restoring mineral content to enamel, addressing early tooth transparency. Topical fluoride applications, calcium phosphate pastes, and specialized toothpaste can encourage mineral uptake.
This method is particularly effective for mild cases, where enamel thinning has not yet exposed dentin. Consistent use strengthens enamel, reduces light penetration, and gradually minimizes translucent areas. Scientific studies highlight that combining fluoride with phosphate compounds can optimize remineralization outcomes and enhance enamel resilience.
In addition to topical treatments, diet modifications support enamel recovery. Incorporating mineral-rich foods and reducing acidic intake prevents further enamel loss and complements tooth transparency remediation efforts.
Treatment Method 2 – Dental Bonding for Tooth Transparency
When tooth transparency progresses beyond mild enamel thinning, dental bonding becomes an effective solution. This method involves applying a tooth-colored resin to the affected area, effectively masking translucent zones. The material is carefully sculpted and hardened using a light-curing process, blending seamlessly with natural enamel.
Dental bonding not only improves aesthetics but also provides a protective layer over weakened enamel. Patients often notice immediate visual improvement, and the procedure is minimally invasive compared to other restorative options. Studies show that properly maintained bonding can last several years, making it a practical choice for moderate transparency.
Bonding is particularly suitable for front teeth, where transparency is most noticeable. Unlike veneers, it requires less enamel removal, preserving natural tooth structure while enhancing appearance. Regular check-ups ensure the bonded material remains intact and continues to support enamel integrity.
Treatment Method 3 – Porcelain Veneers
For severe tooth transparency, porcelain veneers offer a long-lasting cosmetic and protective solution. Veneers are thin ceramic shells custom-made to fit over the tooth surface, covering translucence completely while enhancing shape and color.
Porcelain closely mimics natural enamel, providing a seamless look while offering durability. This treatment is often chosen for patients with extensive enamel loss or aesthetic concerns that cannot be resolved with remineralization or bonding. Scientific reviews suggest that veneers can restore function and appearance for a decade or longer with proper care.
Veneers also provide additional benefits beyond appearance. By covering exposed dentin, they reduce sensitivity and help protect teeth from further wear. While more invasive than bonding, modern veneer techniques preserve as much natural enamel as possible, balancing cosmetic improvement with dental health.
Monitoring and Maintaining Tooth Transparency
Even after treatment, ongoing care is essential for managing tooth transparency. Daily oral hygiene practices, such as gentle brushing and flossing, prevent enamel erosion and maintain overall tooth health. Avoiding excessive acidic foods and beverages helps reduce the risk of recurring translucence.
Regular dental check-ups allow professionals to detect subtle changes in enamel or bonding material. Early intervention ensures that tooth transparency does not worsen and that existing treatments remain effective. Monitoring also provides insight into lifestyle or dietary factors that may contribute to enamel thinning over time.
In addition, using remineralizing toothpaste periodically can support enamel strength even after restorative procedures. Combining preventive care with professional treatments maximizes both aesthetics and tooth longevity.
Lifestyle Adjustments to Reduce Tooth Transparency
Certain habits can exacerbate tooth transparency if not addressed. Limiting acidic food intake, moderating sugar consumption, and drinking water after meals are simple yet effective strategies.
Brushing technique also matters. Using a soft-bristled toothbrush and avoiding excessive force prevents enamel wear. Some studies suggest that spacing brushing sessions to avoid immediately after acidic meals reduces enamel erosion.
Furthermore, nutritional adjustments support enamel health. Foods rich in calcium, phosphorus, and vitamin D help maintain tooth structure, reducing light penetration and enhancing the natural opacity of teeth.
Comparing Treatments for Tooth Transparency
When evaluating tooth transparency solutions, it’s important to consider effectiveness, invasiveness, longevity, and aesthetic outcome. Here’s a clear comparison:
| Treatment Method | Invasiveness | Longevity | Aesthetic Improvement | Protective Effect |
| Remineralization | None | Moderate | Subtle | Supports enamel |
| Dental Bonding | Low | 5–10 years | Moderate to high | Adds protective layer |
| Porcelain Veneers | Moderate | 10+ years | High | Strong protection for dentin |
This table highlights that while remineralization is ideal for early-stage transparency, bonding and veneers are more effective for advanced cases. Choosing a method depends on enamel condition, cosmetic priorities, and long-term maintenance preferences.
Signs Indicating the Need for Professional Evaluation
Recognizing tooth transparency early helps prevent more severe enamel loss. Common indicators include:
- Noticeable translucence near the biting edges of teeth
- Increased sensitivity to hot or cold foods
- Yellowing as the dentin underneath becomes visible
- Rough or thin enamel surfaces
Even if these signs are subtle, consulting a dentist ensures accurate assessment. Early detection allows minimally invasive treatments, potentially avoiding the need for veneers or extensive restorative procedures.
Preventive Strategies to Minimize Tooth Transparency
Preventing tooth transparency revolves around maintaining enamel strength and reducing external stressors. Strategies include:
- Dietary Measures: Limit acidic drinks, sugary foods, and snacking frequency. Include foods rich in calcium, phosphorus, and vitamin D.
- Oral Hygiene Adjustments: Use soft-bristled brushes, avoid aggressive brushing, and choose fluoride or remineralizing toothpaste.
- Lifestyle Habits: Reduce teeth grinding, avoid excessive whitening procedures, and stay hydrated to maintain saliva flow.
By integrating these habits, patients can slow enamel wear and maintain natural opacity, supporting both oral health and aesthetic appearance.
Advanced Scientific Insights on Tooth Transparency
Recent studies suggest that tooth transparency is influenced not just by enamel thickness but by microstructural changes and mineral composition. Research indicates that enamel porosity increases with age, making light pass through more easily. Environmental factors like acidic diets, low pH exposure, and certain medications can accelerate this process.
Innovative treatments under investigation include biomimetic remineralization, which promotes hydroxyapatite deposition to restore enamel density. Early clinical trials suggest this could reduce translucence without invasive procedures, bridging the gap between preventive care and restorative solutions.
Psychological and Aesthetic Implications
Tooth transparency affects more than just oral health it can influence confidence and social interaction. Patients often report self-consciousness about visible edges or color changes. Understanding these psychological aspects is essential when considering treatment options.
Non-invasive and cosmetic procedures, like bonding and veneers, not only restore enamel opacity but also improve self-esteem. By combining functional restoration with aesthetic enhancement, these treatments address both biological and emotional dimensions of tooth transparency.
Final Insights on Tooth Transparency
Understanding tooth transparency requires a multi-faceted approach, blending biology, aesthetics, and lifestyle considerations. Early detection and preventive strategies are key for maintaining enamel integrity. For advanced cases, dental bonding and porcelain veneers offer durable, effective solutions.
By approaching transparency with a combination of scientific insight, personalized care, and lifestyle adjustments, patients can preserve both the health and appearance of their teeth. This holistic understanding ensures that tooth transparency is managed effectively while maintaining natural beauty and functionality.