An impacted tooth is a dental condition that sounds simple at first but becomes surprisingly complex once you look closer. In the first moments of learning about an impacted tooth, many people imagine a tooth that is just “stuck.” In reality, the concept goes much deeper, involving anatomy, growth patterns, genetics, and time. At Livera Clinic, this topic is approached not as a single problem but as a layered biological story where bone, soft tissue, and tooth development interact in fascinating ways.
An impacted tooth is generally described as a tooth that does not erupt into its expected position in the dental arch within the usual timeframe. This does not always mean pain or visible issues. Sometimes, an impacted tooth can remain unnoticed for years, quietly influencing surrounding teeth and bone structures. Understanding how and why this happens allows patients to ask better questions and make informed decisions.
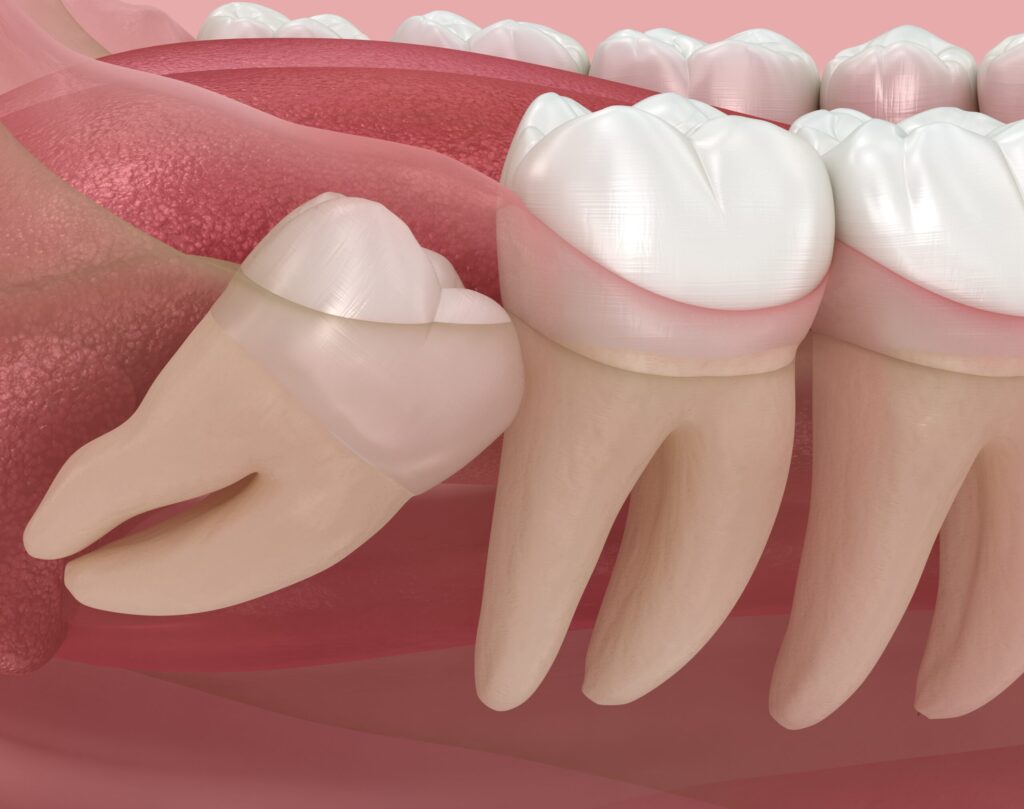
Understanding an Impacted Tooth and Its Biological Background
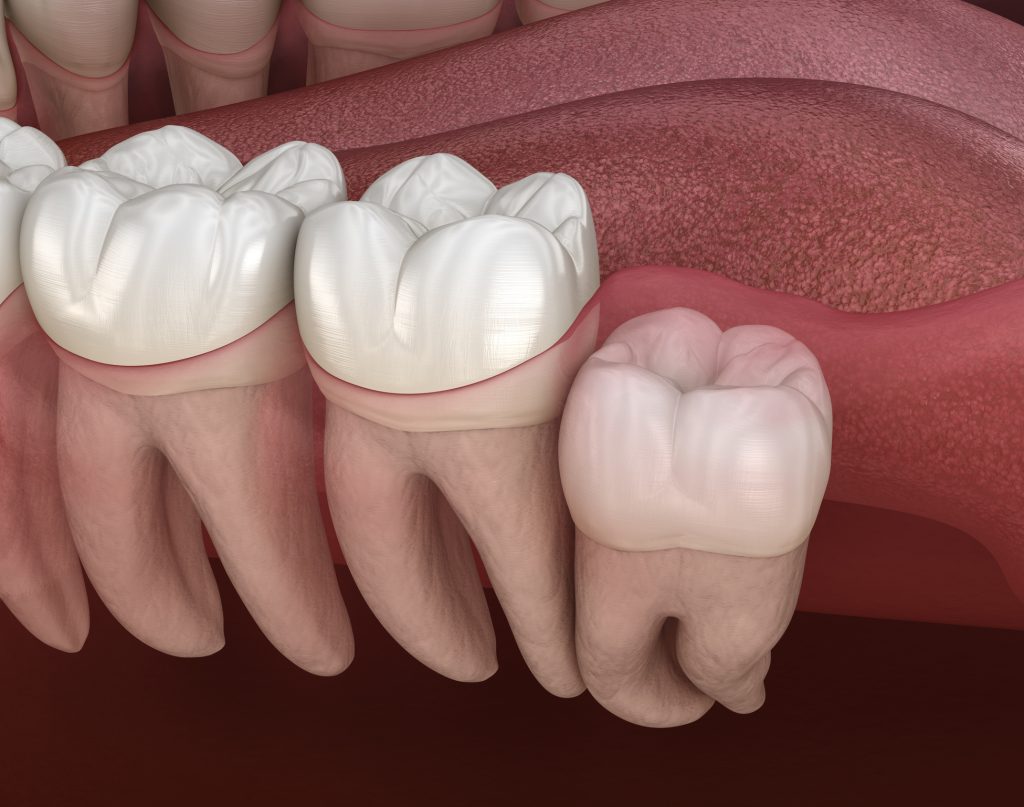
An impacted tooth develops when natural eruption pathways are disrupted. Teeth are designed to follow a biological roadmap from the jawbone to the oral cavity. When this roadmap is blocked, altered, or delayed, the impacted tooth remains partially or fully trapped beneath the gum or bone.
Researchers studying dental eruption patterns suggest that jaw size, tooth size, and evolutionary changes play an important role. Modern jaws are often smaller than those of our ancestors, yet tooth size has not decreased at the same rate. This mismatch creates limited space, making an impacted tooth more likely to occur.
Another important factor is timing. Teeth erupt in a coordinated sequence. When one tooth erupts too early or too late, it can interfere with others. In such scenarios, an impacted tooth is not an isolated issue but part of a broader developmental chain reaction.
Common Types of Impacted Tooth Scenarios
Not every impacted tooth behaves the same way. Dental literature often categorizes an impacted tooth based on position, depth, and orientation. These variations explain why experiences differ from person to person.
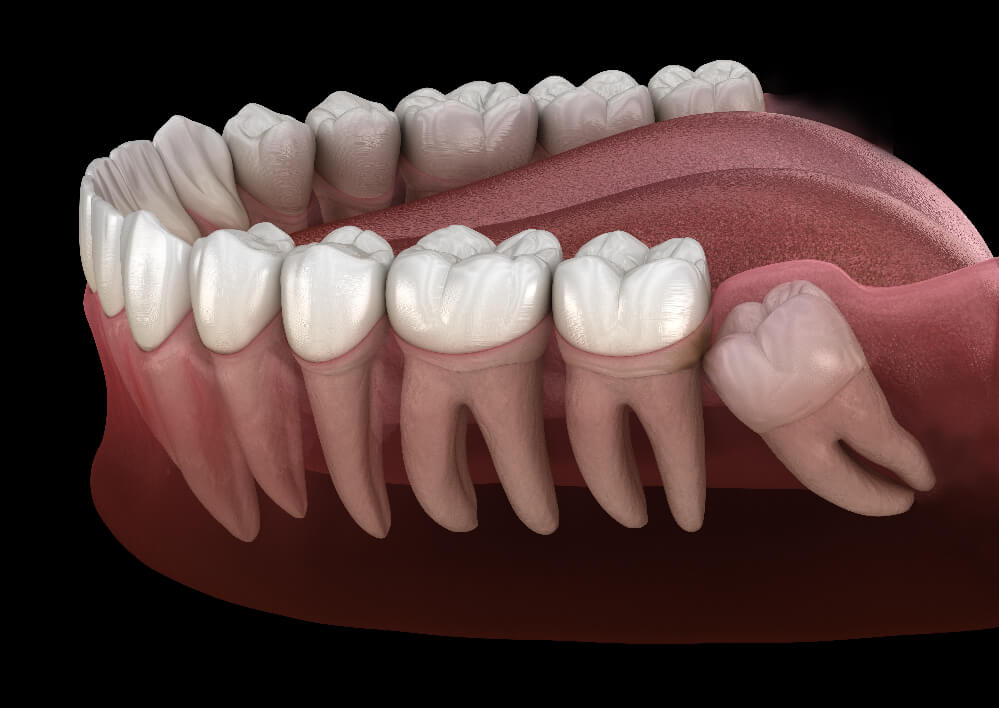
Some impacted teeth remain completely embedded in bone, while others partially emerge through the gum. A tilted impacted tooth may press against adjacent teeth, whereas a vertically positioned one may simply lack the force or space to erupt.
From a clinical observation standpoint, the most frequently discussed impacted teeth are third molars, canines, and premolars. Each type of impacted tooth interacts differently with surrounding tissues, influencing how it is evaluated and monitored over time.
How an Impacted Tooth Is Identified and Evaluated
Identifying an impacted tooth often begins with subtle signs rather than dramatic symptoms. Mild pressure, crowding, or unexplained changes in bite alignment can all be indirect clues. In many cases, an impacted tooth is discovered incidentally during routine imaging.
Dental imaging technologies allow professionals to observe the exact position of an impacted tooth relative to nerves, sinuses, and adjacent roots. These visual insights transform an abstract concept into a clear anatomical map.
Evaluation does not focus only on the tooth itself. The surrounding bone density, gum condition, and neighboring teeth are all considered. This broader assessment explains why an impacted tooth is often discussed as part of an oral ecosystem rather than a standalone issue.
Impacted Tooth Surgery and How the Procedure Is Approached
When people hear about impacted tooth surgery, they often imagine a single standardized procedure. In reality, the surgical approach varies significantly depending on the depth, angle, and location of the impacted tooth.
The process typically begins with detailed planning. Imaging data is analyzed to understand access points and tissue relationships. For a deeply embedded impacted tooth, bone removal may be part of the approach, while a partially erupted impacted tooth may require less structural modification.
From a technical perspective, impacted tooth surgery focuses on precision rather than force. Modern techniques emphasize controlled movements that respect surrounding tissues. This careful approach reflects how an impacted tooth is treated as part of a living structure, not just an object to be removed.
Healing, Adaptation, and the Body’s Response After Impacted Tooth Surgery
After an impacted tooth procedure, the body enters a complex healing phase. This process involves bone remodeling, soft tissue adaptation, and cellular repair. Rather than viewing healing as a passive waiting period, many researchers describe it as an active biological dialogue.
Bone cells reorganize around the former position of the impacted tooth, gradually reshaping the jaw structure. Gum tissue also adapts, forming a new seal that protects underlying bone. These changes occur in stages, influenced by individual biology and environmental factors.
Interestingly, studies show that the body often compensates remarkably well after the removal of an impacted tooth. Adjacent teeth may subtly shift, and bite forces redistribute themselves over time. This adaptability highlights the resilience of oral structures.
Long Term Considerations Related to an Impacted Tooth
An impacted tooth is not only about the present moment but also about long term dynamics. Even when asymptomatic, an impacted tooth can influence neighboring teeth, jaw alignment, and bone density over many years.
In some cases, pressure from an impacted tooth contributes to crowding or root resorption in adjacent teeth. In others, the surrounding follicular tissue may change over time. These possibilities explain why monitoring an impacted tooth is often discussed in long term dental planning.
From an analytical perspective, an impacted tooth serves as a reminder that oral health evolves continuously. Decisions are rarely binary and often involve weighing structural, functional, and biological factors together.
Scientific Insights and Research Trends Around Impacted Tooth Cases
Academic interest in the impacted tooth phenomenon has increased as imaging and data analysis tools improve. Recent observational studies explore correlations between impacted tooth patterns and craniofacial growth trends across populations.
Some research suggests that dietary softness over generations may contribute to reduced jaw stimulation during growth, indirectly increasing the likelihood of an impacted tooth. Other analyses examine genetic markers that influence eruption timing and tooth orientation.
These insights do not present absolute conclusions but offer intriguing frameworks. Viewing an impacted tooth through a scientific lens transforms it from a simple dental issue into a reflection of human evolution, lifestyle, and biology.
Rethinking the Impacted Tooth as a Broader Concept
An impacted tooth is more than a tooth that fails to emerge. It is a result of timing, space, genetics, and adaptation. From initial development to potential surgical considerations, the story of an impacted tooth unfolds across years, sometimes decades.
By understanding how an impacted tooth forms, how it is evaluated, and how the body responds, individuals gain a clearer perspective. At Livera Clinic, this topic is framed not as a problem to fear but as a condition to understand.
When viewed holistically, an impacted tooth becomes a fascinating example of how the human body balances structure and function, even when the original plan changes.