Gum Disease is one of those oral health topics that almost everyone has heard of, yet very few people truly understand in depth. At first glance, it may seem like a simple issue related to brushing habits. In reality, Gum Disease is a multifactorial condition shaped by biology, lifestyle, environment, and even psychology. At Livera Clinic, this topic is approached not as a narrow dental problem, but as a complex biological process that reflects how the body interacts with bacteria over time.
The Biological Foundation of Gum Disease
At its core, Gum Disease begins with a biological imbalance. The human mouth hosts hundreds of bacterial species, most of which are harmless or even beneficial. Problems arise when this delicate ecosystem shifts.
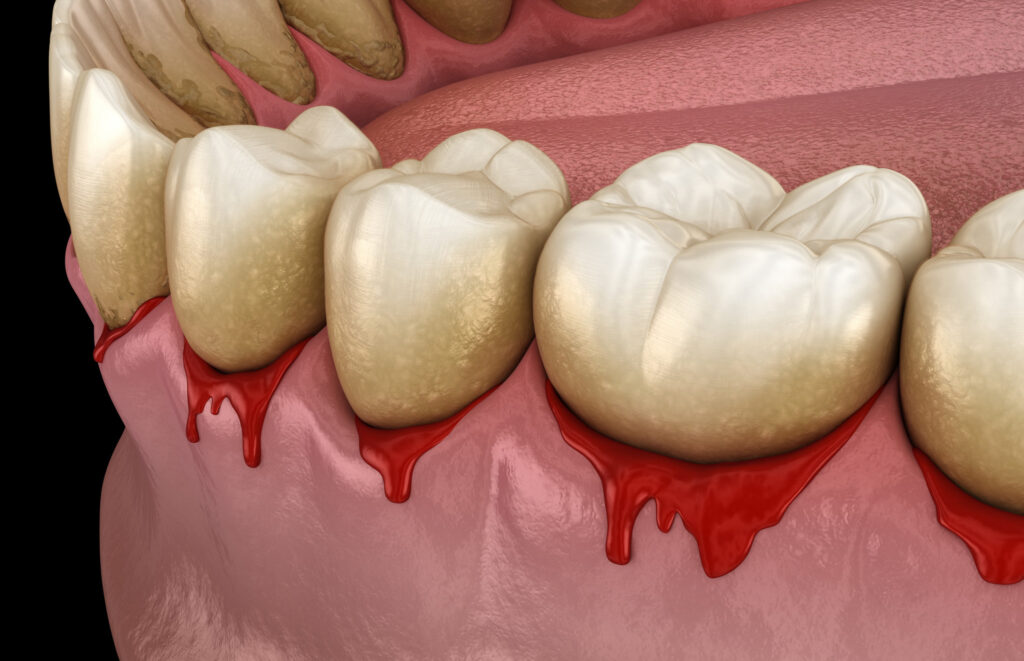
When bacterial communities grow unchecked along the gum line, they form biofilms that are difficult to remove. Over time, these biofilms interact with the immune system. In the early stages of Gum Disease, the body responds with inflammation as a defensive reaction rather than an infection itself.
What makes this process fascinating is that tissue damage is often caused more by the body’s inflammatory response than by bacteria alone. This explains why Gum Disease can progress differently from one person to another, even when similar bacterial profiles are present.
How Dental Plaque Contributes to Gum Disease
Dental plaque is frequently mentioned in discussions about Gum Disease, but its role is often oversimplified. Plaque is not just food debris. It is a living microbial structure.
As plaque matures, oxygen levels decrease, allowing anaerobic bacteria to thrive. These bacteria are strongly associated with advanced stages of Gum Disease. Their metabolic byproducts interact with gum tissues and trigger immune responses that lead to swelling, redness, and gradual tissue breakdown.
Interestingly, plaque alone does not automatically cause Gum Disease. Research suggests that susceptibility varies. Some individuals develop significant inflammation with minimal plaque, while others show little response despite heavy buildup. This variation highlights the importance of host response rather than plaque quantity alone.
Genetic and Hereditary Factors in Gum Disease
One of the most compelling areas of modern research focuses on genetic predisposition. Gum Disease is not inherited directly, but genetic traits can influence how the immune system reacts to bacterial challenges.
Certain genetic markers are linked to exaggerated inflammatory responses. In individuals carrying these traits, Gum Disease may progress faster and appear at a younger age. This does not mean the condition is inevitable, but it does help explain why some families report similar gum problems across generations.
From a scientific perspective, genetics act as a volume control. They do not create the bacteria responsible for Gum Disease, but they influence how loudly the body reacts to them.
Lifestyle Habits That Influence Gum Disease Development
Lifestyle choices play a subtle yet powerful role in shaping the oral environment. Habits such as smoking, stress exposure, and dietary patterns have all been associated with changes in how Gum Disease develops.
Smoking, for example, alters blood flow in gum tissues. This may reduce visible signs of inflammation, making Gum Disease harder to detect in early stages. At the same time, immune responses become less effective, allowing deeper tissue damage to occur silently.
Chronic stress introduces another layer. Stress hormones can influence immune regulation, which in turn affects how the body responds to oral bacteria. Over long periods, this altered response may contribute to the persistence of Gum Disease, even in individuals with otherwise good oral hygiene.

Hormonal Changes and Their Link to Gum Disease
Hormones are chemical messengers, and gum tissues are highly sensitive to them. Fluctuations during puberty, pregnancy, and menopause have all been linked to temporary changes in gum health.
During these periods, blood flow to the gums can increase, making tissues more reactive to plaque. This heightened sensitivity does not cause Gum Disease by itself, but it can amplify existing inflammatory responses.
What makes hormonal influence particularly interesting is its reversibility. In many cases, gum inflammation linked to hormonal changes stabilizes once hormone levels return to baseline. However, if bacterial triggers remain present, this temporary imbalance can evolve into chronic Gum Disease.
Systemic Conditions Associated with Gum Disease
The relationship between oral health and overall health has been a major focus of scientific research. Gum Disease has been associated with various systemic conditions, not as a direct cause, but as a condition that shares inflammatory pathways.
Metabolic disorders, immune system dysregulation, and vascular conditions have all been studied in relation to Gum Disease. In these cases, chronic inflammation appears to be the common denominator.
Rather than viewing Gum Disease as an isolated problem, many researchers now see it as part of a broader inflammatory profile. This perspective has reshaped how dental science understands the significance of gum health within the body.
Environmental and Behavioral Triggers of Gum Disease
Beyond biology and genetics, everyday behaviors influence the risk profile of Gum Disease. Irregular oral hygiene routines, limited access to preventive care, and even sleep patterns can alter bacterial balance.
Nighttime dry mouth, for example, reduces saliva flow. Saliva plays a key role in neutralizing acids and washing away bacteria. Reduced saliva can create conditions that favor the progression of Gum Disease over time.
Environmental exposure, such as air quality and occupational stress, has also been explored. While these factors are indirect, they contribute to systemic stress responses that may influence oral inflammation.
Why Gum Disease Progresses Silently
One of the defining characteristics of Gum Disease is its ability to advance without noticeable pain. This silent progression is not accidental.
Gum tissues adapt gradually to chronic inflammation. Nerve endings may become less responsive, and symptoms like bleeding may be dismissed as minor. This makes Gum Disease fundamentally different from acute dental problems that demand immediate attention.
From a scientific standpoint, this silent nature explains why advanced gum conditions are often discovered incidentally rather than through discomfort.
The Long Term Biological Impact of Gum Disease
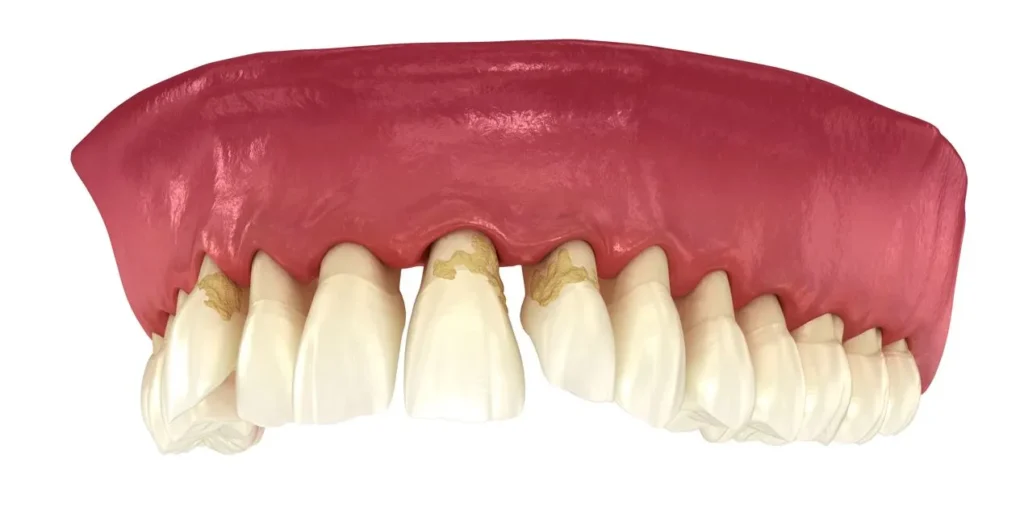
As Gum Disease advances, structural changes occur within the supporting tissues of the teeth. Collagen fibers degrade, bone remodeling patterns shift, and microbial communities become more specialized.
These changes are not sudden events. They represent the cumulative result of years of interaction between bacteria and host response. Understanding this timeline is essential to grasp why Gum Disease is considered a chronic condition rather than a temporary one.
This long term perspective also explains why early stages often go unnoticed, while later stages appear complex and resistant to change.
Gum Disease as a Research Driven Topic in Modern Dentistry
Few dental topics have generated as much research as Gum Disease. From microbiology to immunology, it sits at the crossroads of multiple scientific disciplines.
At Livera Clinic, this condition is viewed not only as a clinical concern but also as an evolving research field. New studies continue to reshape how professionals understand bacterial behavior, host response, and tissue regeneration in relation to Gum Disease.
This ongoing research ensures that the topic remains dynamic rather than static, with new insights emerging regularly.
Understanding What Causes Gum Disease
Understanding what causes Gum Disease requires stepping beyond surface level explanations. It is not simply about brushing habits or plaque presence. It is about how the body responds to long term microbial challenges under the influence of genetics, lifestyle, hormones, and systemic health.
By examining Gum Disease through a comprehensive lens, it becomes clear why it remains one of the most discussed and researched topics in oral science. Awareness begins with understanding causes, and understanding creates a foundation for informed decisions.