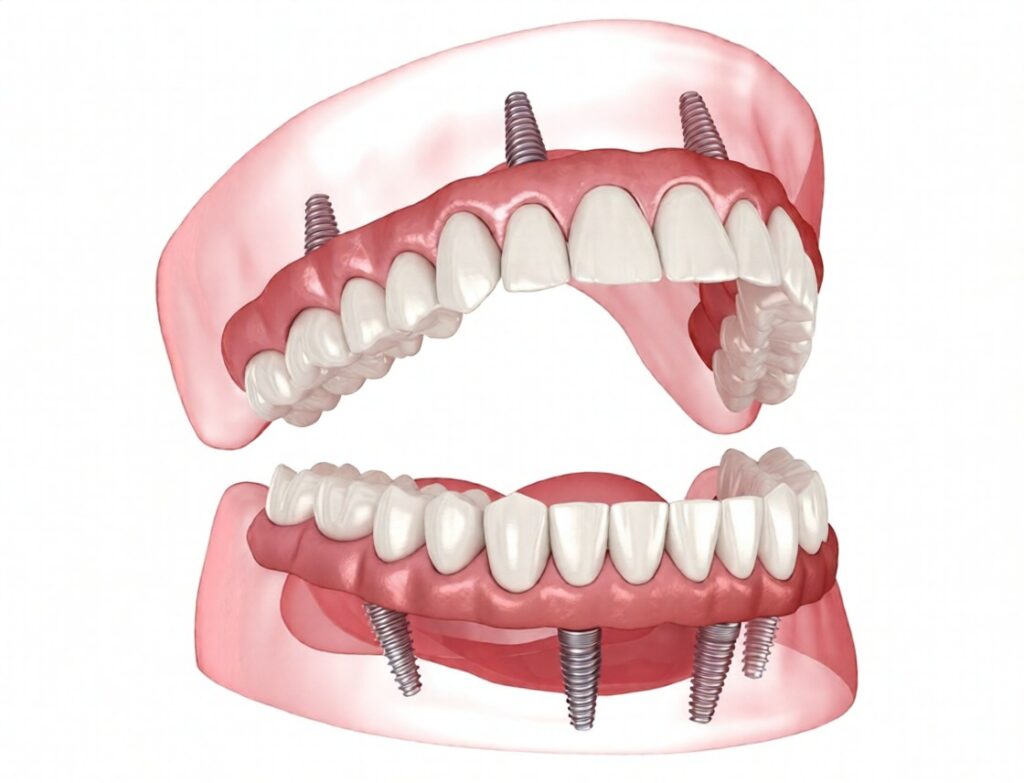
The journey of Dental Implants is not just about placing a titanium post into the jawbone. It is a carefully orchestrated biological process where bone, soft tissue, and time work together to create a stable and functional tooth replacement. Understanding the healing stages of Dental Implants can help patients better interpret what is happening beneath the surface and why patience is a critical part of the process.
At Livera Clinic, this process is viewed not as a single procedure, but as a sequence of healing phases influenced by biology, technique, and individual variability. While timelines may differ, the core stages of healing in Dental Implants follow a predictable pattern supported by clinical research and long-term observations.
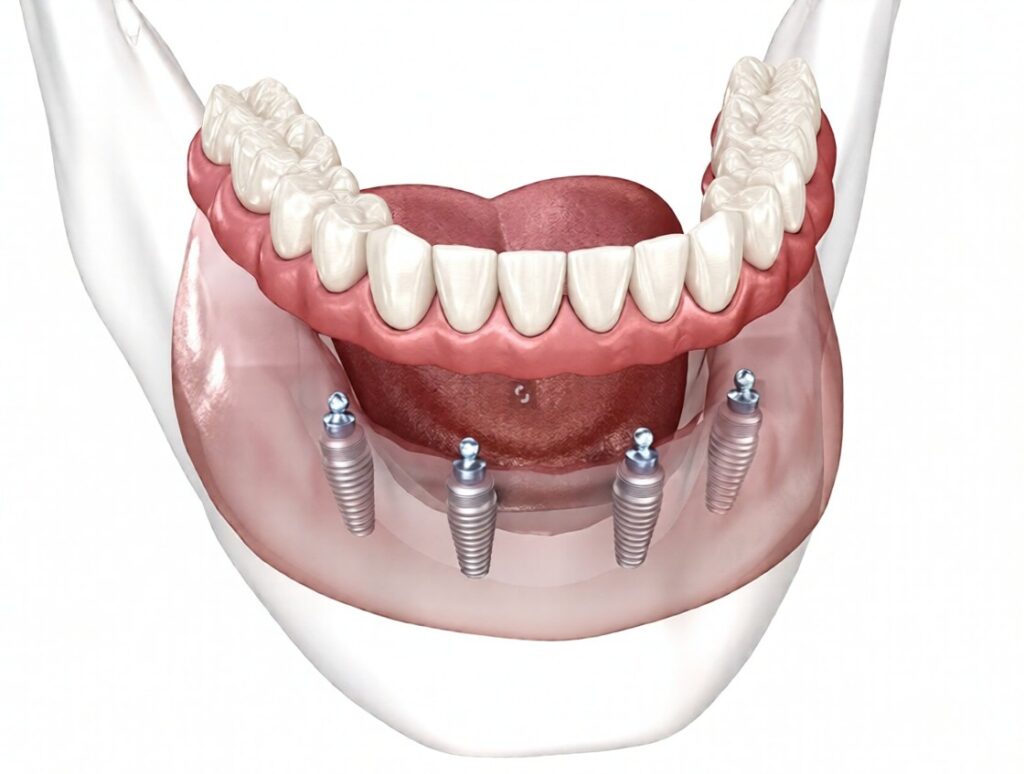
Initial Healing After Dental Implants Placement
The first stage begins immediately after the surgical placement of Dental Implants. During this phase, the body initiates its natural wound-healing response. Blood clot formation occurs around the implant site, acting as a biological scaffold for incoming cells.
Within the first few days, inflammatory cells migrate to the area. This is not a negative process; rather, it is essential for cleaning the site and preparing it for tissue regeneration. Patients may notice mild swelling or sensitivity, which reflects this biological activity.
Over the next one to two weeks, soft tissue begins to close around the implant. The gum tissue gradually stabilizes, forming a protective seal. This stage sets the foundation for deeper healing processes that follow.
Osseointegration: The Core of Dental Implants Healing
Osseointegration is often considered the most critical phase in the success of Dental Implants. This process refers to the direct structural and functional connection between the implant surface and the surrounding bone.
At a microscopic level, bone cells begin to attach to the implant surface. Over time, these cells proliferate and form new bone tissue, effectively anchoring the implant in place. This process can take several weeks to several months, depending on factors such as bone density and overall health.
Interestingly, modern implant surfaces are designed to enhance osseointegration. Textured or treated surfaces can increase the surface area, allowing more bone contact and potentially improving stability. However, this does not eliminate the biological timeline required for proper healing.
Bone Remodeling Around Dental Implants
Once initial osseointegration begins, the body enters a phase known as bone remodeling. During this stage, the newly formed bone is continuously reshaped and strengthened.
Bone is a dynamic tissue. It responds to mechanical forces and adapts accordingly. Around Dental Implants, this means that the bone structure becomes more organized and capable of supporting functional loads.
This phase may extend over several months. The implant becomes increasingly stable, transitioning from primary stability, achieved mechanically during placement, to secondary stability, achieved biologically through bone regeneration.
Soft Tissue Adaptation in Dental Implants
While bone healing is crucial, the role of soft tissue should not be underestimated in Dental Implants success. The gums form a barrier that protects the underlying bone and implant from external factors.
During this stage, the gum tissue adapts to the shape of the implant and any temporary or permanent restorations. A well-adapted soft tissue seal helps reduce the risk of bacterial infiltration.
Clinically, the appearance of the gums becomes more natural over time. Color, contour, and firmness gradually resemble the surrounding tissues. This contributes not only to function but also to aesthetic outcomes.
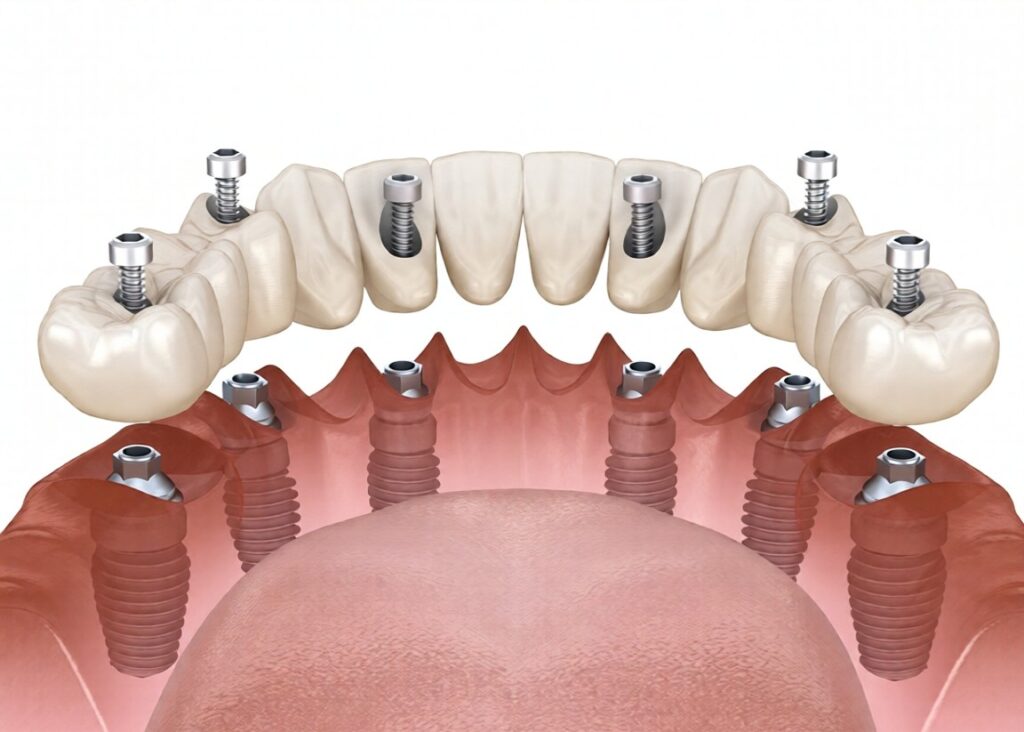
Functional Loading Phase of Dental Implants
After sufficient healing, Dental Implants enter the functional loading phase. This is when the implant begins to support a crown, bridge, or denture.
Functional loading introduces controlled mechanical forces to the implant. These forces stimulate further bone adaptation, reinforcing the connection between the implant and the jawbone.
However, timing is critical. Premature loading may interfere with osseointegration, while delayed loading may prolong treatment unnecessarily. Clinicians evaluate stability and healing progress before moving to this stage.
Long-Term Maintenance of Dental Implants
Healing does not truly end once the implant is restored. Instead, Dental Implants require ongoing maintenance to preserve their stability and function.
Over time, the surrounding tissues continue to respond to environmental and mechanical factors. Regular monitoring helps identify any changes in bone levels or soft tissue health.
Studies suggest that long-term success is closely linked to consistent care and professional follow-up. While Dental Implants are designed to be durable, they remain part of a living biological system that evolves over time.
Factors Influencing Healing in Dental Implants
Healing is not identical for every patient. Several factors can influence how quickly and effectively Dental Implants integrate with the body.
Key variables include:
- Bone density and volume
- General health and metabolic conditions
- Surgical technique and implant design
- Oral hygiene and post-operative care
- Lifestyle factors such as smoking
Each of these elements interacts with the biological processes described earlier. For example, higher bone density may support faster osseointegration, while certain conditions may slow tissue regeneration.
Timeline Overview of Dental Implants Healing
Below is a simplified overview of the typical healing timeline associated with Dental Implants:
| Healing Stage | Approximate Duration | Biological Activity |
| Initial Healing | 1 to 2 weeks | Soft tissue closure, inflammation response |
| Early Osseointegration | 2 to 6 weeks | Bone cell attachment begins |
| Advanced Osseointegration | 6 weeks to 3 months | Bone formation and strengthening |
| Bone Remodeling | 3 to 6 months and beyond | Structural adaptation of bone |
| Functional Loading | After 3 to 6 months | Implant begins supporting prosthetics |
It is important to note that these timelines are approximate and may vary significantly between individuals.
Scientific Insights into Dental Implants Healing
Research in implant dentistry continues to explore how materials, surface technologies, and biological factors influence healing. For example, studies on implant surface roughness have shown improved bone-to-implant contact ratios.
Additionally, advancements in imaging technologies allow clinicians to monitor healing more precisely. Three-dimensional imaging provides insights into bone density changes and implant stability over time.
Another area of interest is the role of growth factors and biomaterials in enhancing healing. While these approaches show promise, they are still being evaluated in long-term clinical contexts.
The healing process of Dental Implants is a complex and dynamic interaction between biology and technology. From initial tissue response to long-term bone adaptation, each stage contributes to the overall success of the implant.
At Livera Clinic, understanding these stages allows for a more informed and patient-centered approach. While the process requires time, it reflects the body’s remarkable ability to integrate artificial structures into its natural framework.
Ultimately, Dental Implants are not just a replacement for missing teeth; they represent a collaboration between science and the human body, unfolding gradually through carefully coordinated healing stages.