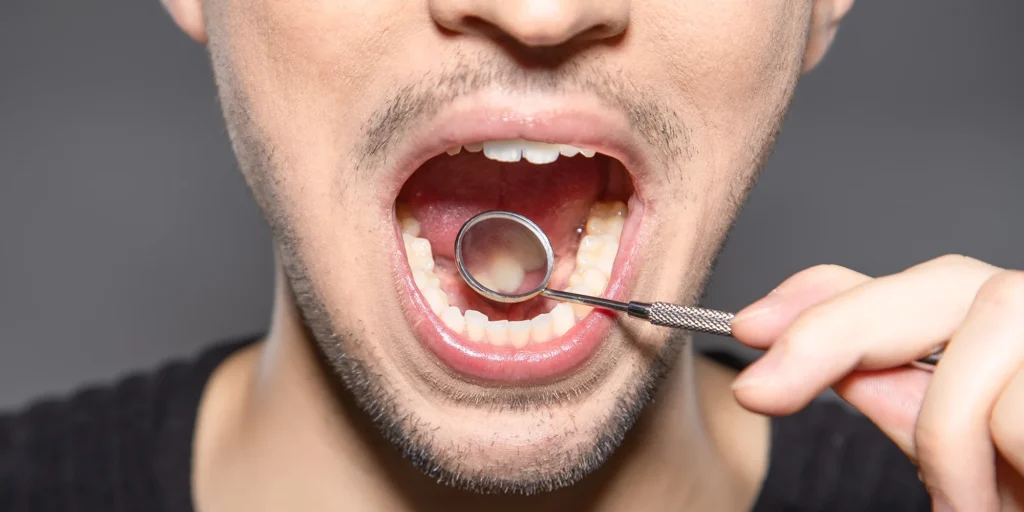
Experiencing dry mouth can be more than a minor inconvenience. Medically known as xerostomia, dry mouth occurs when the salivary glands fail to produce enough saliva to keep the mouth adequately moist. While it may seem trivial, the consequences of persistent dry mouth range from difficulty speaking and swallowing to increased risk of dental issues. Understanding what triggers this condition is essential for anyone curious about oral health, hydration, and the body’s intricate biochemical balance.
How Saliva Production Works
Saliva is often underestimated despite its critical role in maintaining oral health. Composed mainly of water, electrolytes, enzymes, and proteins, saliva lubricates the mouth, initiates digestion, and protects teeth from decay. Dry mouth arises when the delicate mechanism controlling saliva secretion is disrupted.
Saliva is produced by three major pairs of salivary glands the parotid, submandibular, and sublingual glands along with hundreds of minor glands scattered across the mouth and throat. Nerve signals from the autonomic nervous system regulate their activity, meaning stress, fatigue, or neurological conditions can inadvertently reduce saliva flow.
Common Medications That Trigger Dry Mouth
One of the leading causes of dry mouth is medication. According to multiple studies, over 400 commonly prescribed drugs can decrease saliva production. These include:
- Antihistamines: Often used for allergies, they reduce nasal and oral secretions.
- Antidepressants: Selective serotonin reuptake inhibitors (SSRIs) and tricyclic antidepressants frequently list dry mouth as a side effect.
- Blood pressure medications: Diuretics and beta-blockers may indirectly decrease hydration levels, contributing to reduced saliva.
Interestingly, the effect is dose-dependent. Higher doses or long-term usage can intensify the dryness sensation, creating a feedback loop where discomfort encourages less fluid intake, further worsening the problem.
Systemic Conditions Linked to Dry Mouth
Beyond medications, certain systemic conditions are closely tied to chronic dry mouth. These include autoimmune disorders, metabolic syndromes, and neurological diseases:
- Sjogren’s Syndrome: An autoimmune disorder that primarily attacks the salivary and tear glands, causing persistent dryness.
- Diabetes: High blood sugar levels may impair salivary gland function and reduce moisture in the mouth.
- Parkinson’s Disease: Neurodegenerative conditions can alter nerve signals to salivary glands, resulting in xerostomia.
Research indicates that when dry mouth stems from systemic illness, it often presents alongside other symptoms, such as fatigue, blurred vision, or digestive issues, highlighting the interconnected nature of bodily systems.

Lifestyle Factors Contributing to Dry Mouth
Several lifestyle choices can exacerbate or trigger dry mouth. Alcohol and caffeine consumption, tobacco use, and insufficient water intake are frequent contributors.
For example, alcohol is a diuretic that promotes fluid loss, while caffeine can temporarily inhibit salivary secretion. Smoking or chewing tobacco not only dries oral tissues but also introduces chemicals that irritate salivary glands, creating longer-term dysfunction. Even mouth breathing during sleep—common in people with nasal congestion—can accelerate oral dryness.
Environmental and Seasonal Influences
Interestingly, dry mouth isn’t only a personal issue; the environment plays a significant role. Low humidity, heated indoor spaces, and extreme cold can reduce moisture levels in the mouth. Seasonal changes also matter: winter months with artificial heating or summer heat waves without adequate hydration can increase the frequency and severity of dry mouth episodes.
Environmental triggers are often overlooked, yet they can explain why some individuals notice dryness only at specific times of the year or in certain settings.
How Age Affects Saliva Production
Aging naturally affects salivary gland function. Studies suggest that people over 60 are more likely to experience dry mouth, not necessarily because of age alone, but due to higher medication use, chronic illnesses, and changes in tissue elasticity.
Saliva production may decline subtly over decades, making early recognition of dryness essential. Older adults may confuse this sensation with simple thirst, but untreated dry mouth can lead to complications like dental erosion, infections, and difficulties in speech or swallowing.
Innovative Research and Emerging Insights
Recent studies have begun exploring less obvious contributors to dry mouth. For instance, microbiome imbalances in the oral cavity might influence saliva consistency and flow. Similarly, hormonal fluctuations, especially in women during menopause, have been linked to increased incidence of xerostomia.
Emerging therapies, such as targeted gland stimulation and saliva substitutes enriched with enzymes, offer promising avenues for mitigating dry mouth beyond traditional remedies. While these innovations are still under investigation, they highlight how complex and multifaceted saliva regulation truly is.
Connecting the Dots on Dry Mouth
Dry mouth is far from a simple nuisance. It represents a convergence of physiological, environmental, and lifestyle factors. From medications and systemic illnesses to seasonal influences and aging, understanding the underlying causes provides a broader perspective on oral health and hydration.
Awareness is the first step. Observing when dry mouth occurs, what triggers it, and how it affects daily life can inform discussions with healthcare professionals, researchers, or even curious readers seeking to understand the body’s complex chemistry. By appreciating the science behind saliva, we can better grasp why this small yet essential fluid profoundly impacts health and well-being.