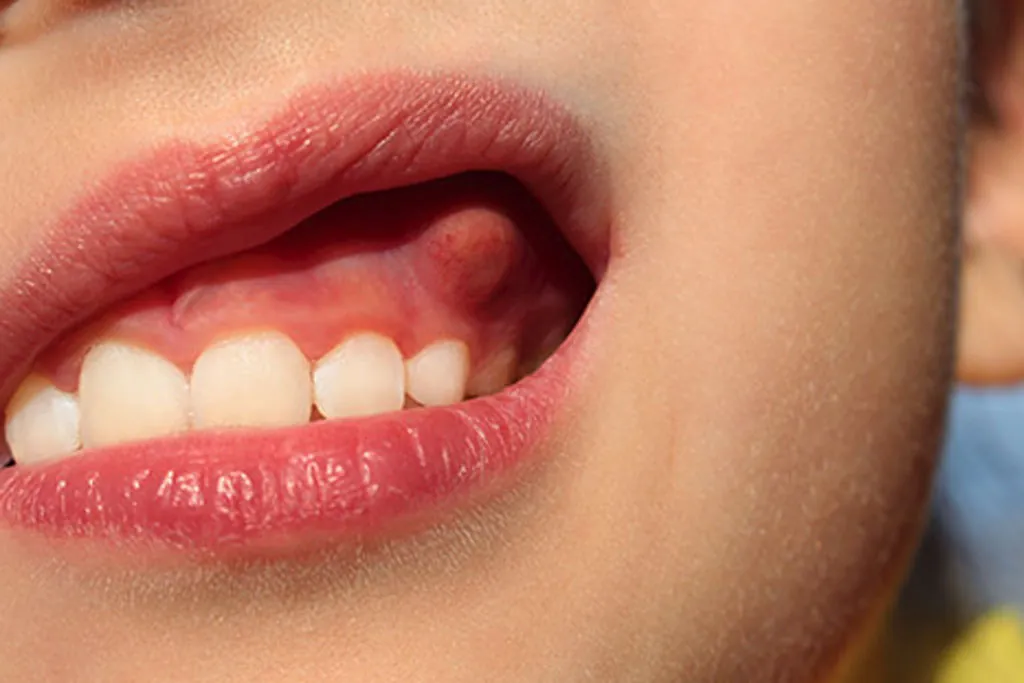
Dental abscess is a phrase that often sounds clinical and distant, yet the experience behind it is anything but abstract. For many people, it begins with a subtle discomfort that feels easy to ignore, only to grow into something far more demanding of attention. This first part explores what a dental abscess actually is, how it forms, and why it has such a strong presence in both medical discussions and everyday concerns.
At its core, a dental abscess refers to a localized collection of fluid and bacteria that develops when the balance inside the mouth is disrupted. The mouth is a complex ecosystem, constantly negotiating between bacteria, saliva, enamel, and soft tissue. When that balance shifts, pressure builds. Understanding this process helps explain why a dental abscess is not just about teeth, but about systems interacting over time.
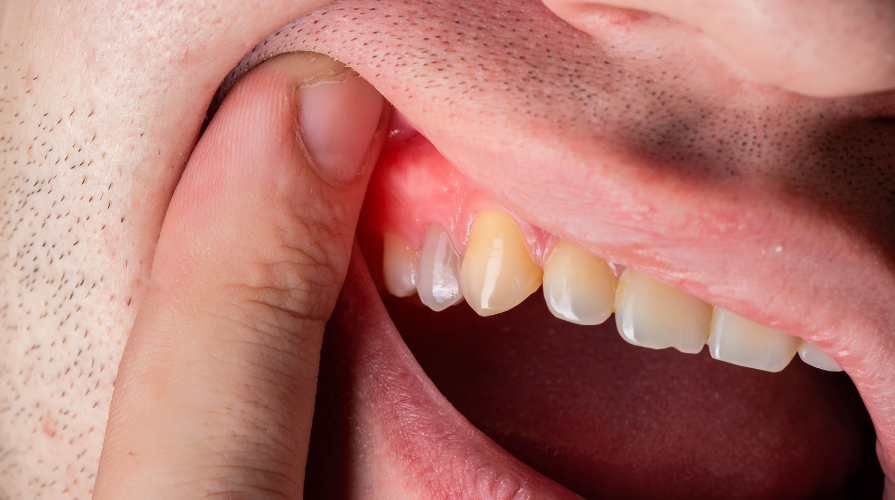
Understanding Dental Abscess as a Biological Process
A dental abscess does not appear suddenly. It is usually the outcome of a slow biological conversation between bacteria and the body’s defense mechanisms. Small openings, whether from decay, cracks, or gum irritation, allow bacteria to travel deeper than they normally would.
Once bacteria settle in an area with limited circulation, the body responds by sending immune cells. This response creates fluid and pressure. Over time, this enclosed reaction space becomes what people recognize as a dental abscess. It is less an event and more a process unfolding quietly before becoming noticeable.
Interestingly, not every bacterial presence leads to a visible outcome. What makes a dental abscess distinct is the combination of confinement and immune response. Without space to drain or disperse, the area becomes concentrated, making sensations more intense and persistent.
Why Dental Abscess Develops Beneath the Surface
One reason a dental abscess draws attention is because much of its activity happens out of sight. Teeth and gums appear solid, but beneath them lies a network of canals, tissues, and microscopic pathways. These spaces can carry signals of discomfort long before visible signs appear.
From a biological perspective, the body often tolerates low level irritation. It prioritizes stability over immediate reaction. This is why a dental abscess may exist for a while before it becomes impossible to ignore. The escalation usually reflects a threshold being crossed rather than a sudden change.
This hidden progression also explains why people often describe confusion when symptoms intensify. The source feels unclear because the process itself has been gradual and internal. In this sense, a dental abscess challenges the assumption that visible problems always announce themselves early.
Different Patterns Within Dental Abscess Formation
Although the term dental abscess is used broadly, it can describe different patterns depending on where the fluid collects. Some develop closer to the tooth structure, while others form along the surrounding tissue. These variations influence how the body perceives and responds to the condition.
What they share is a similar logic. Restricted space, bacterial presence, and immune activity combine to create pressure. This pressure is what makes a dental abscess feel distinctive compared to other oral issues. It is not just irritation, but containment.
Researchers often describe this as a feedback loop. The more confined the area, the more intense the immune response becomes. This loop explains why a dental abscess can feel persistent rather than fleeting.
Dental Abscess and the Language of Sensation
People often struggle to describe what a dental abscess feels like because it does not behave consistently. Sensations may fluctuate, intensify, or temporarily fade. This variability reflects changes in pressure rather than resolution.
From a sensory standpoint, the body interprets pressure differently than surface irritation. That is why a dental abscess can feel deep, dull, or throbbing rather than sharp. These signals are the nervous system’s way of communicating internal tension.
Understanding this sensory language helps demystify the experience. A dental abscess is not random discomfort. It is structured, patterned, and responsive to changes inside the tissue environment.
Why Dental Abscess Becomes a Repeated Topic
The reason dental abscess appears so frequently in discussions is not only its physical impact, but its symbolic one. It represents how small, overlooked changes can grow into complex situations. This makes it relatable beyond dentistry.
In everyday conversations, a dental abscess often becomes shorthand for something that escalates quietly. Scientifically, it serves as an example of how systems react under constraint. Both perspectives contribute to its lasting presence in public awareness.
This first part sets the stage by framing a dental abscess not as an isolated issue, but as a biological narrative. In the next part, the focus will shift toward how this condition is recognized, interpreted, and understood through observation rather than intervention.
Understanding the Nature of a dental abscess
A dental abscess is often described as a localized pocket of infection, but that definition barely captures its complexity. Beneath the surface, a dental abscess represents an ongoing interaction between bacteria, the immune system, and dental structures. It usually forms when bacteria gain access to deeper layers of the tooth or surrounding tissue, often through decay, cracks, or previous dental work.
What makes a dental abscess particularly interesting is that it is not a sudden event. It develops gradually. Long before pain appears, microscopic changes begin inside the tooth. Bacteria multiply, pressure builds, and the body responds with inflammation. This silent phase explains why many people are surprised when symptoms finally appear.
From a biological perspective, a dental abscess is the body’s attempt to contain infection. Pus forms as immune cells gather to isolate harmful bacteria. While this response is protective, it also creates pressure, which contributes to discomfort and swelling.
How a dental abscess forms over time
The formation of a dental abscess follows a logical sequence rather than a random pattern. It often starts with tooth decay that reaches the pulp, the inner part of the tooth containing nerves and blood vessels. Once bacteria enter this space, they gain access to a rich environment that supports rapid growth.
As the infection progresses, the body reacts by sending white blood cells to the area. These cells, along with bacteria and damaged tissue, accumulate as pus. Over time, this buildup seeks an outlet, leading to the formation of an abscess near the root of the tooth or in the surrounding gum tissue.
Interestingly, not all dental abscess cases feel the same. Some progress slowly with mild symptoms, while others escalate quickly. This variation depends on factors such as immune response, bacterial type, and the structure of the tooth itself.
Types of dental abscess and how they differ
Not every dental abscess originates in the same place. Clinically, abscesses are often categorized based on their location. Each type follows a slightly different path and creates distinct sensations.
A periapical abscess develops at the tip of the tooth root. It is commonly linked to untreated cavities or trauma. A periodontal abscess, on the other hand, forms in the gums and is often associated with gum disease. There is also the gingival abscess, which remains limited to gum tissue without involving the tooth itself.
Despite these differences, all forms of dental abscess share one core feature: trapped infection. Understanding the type helps explain why symptoms may vary and why the experience feels different from one person to another.
Symptoms that shape the experience of a dental abscess
The symptoms of a dental abscess are not limited to pain. While discomfort is common, many people first notice pressure, sensitivity, or swelling. These sensations may fluctuate, sometimes easing temporarily before returning more intensely.
A distinctive aspect of a dental abscess is how symptoms can radiate. Pain may extend to the jaw, ear, or neck, creating confusion about the source. In some cases, a foul taste or odor appears when the abscess begins to drain on its own.
It is also worth noting that symptoms do not always correlate with severity. A relatively small dental abscess can feel intense, while a larger one may remain surprisingly subtle for a time. This unpredictability is part of what makes the condition so widely discussed.
Why a dental abscess sometimes feels like it disappears
One of the most puzzling aspects of a dental abscess is the way symptoms can fade temporarily. This often happens when pressure is relieved, either through spontaneous drainage or reduced inflammation. When this occurs, people may assume the problem has resolved.
In reality, the underlying infection often remains. The temporary relief is not a cure but a shift in pressure dynamics. The bacteria can persist, continuing their activity beneath the surface even when discomfort subsides.
This cycle of flare up and calm contributes to misunderstanding around how a dental abscess truly goes away. The absence of pain does not necessarily indicate resolution. Instead, it reflects a change in how the body and infection are interacting at that moment.
The broader biological story behind a dental abscess
Beyond teeth and gums, a dental abscess illustrates how the body negotiates with infection. It shows the balance between containment and escalation. The immune system works to isolate bacteria, but structural limits within the mouth create pressure points.
From an anatomical standpoint, teeth are rigid structures with limited space. When inflammation occurs inside them, there is nowhere for swelling to expand. This constraint is a key reason why a dental abscess produces such distinctive sensations compared to infections elsewhere in the body.
Understanding this broader biological context helps explain why a dental abscess is remembered not just as a dental issue, but as a vivid physical experience. It is the combination of confined anatomy, immune response, and bacterial activity that gives the condition its unique character.
How people believe a dental abscess goes away
When people ask how a dental abscess goes away, they are often describing an experience rather than a medical process. The most common belief is that pain relief equals resolution. If swelling decreases or discomfort fades, it feels logical to assume the issue has ended.
This belief is reinforced by how the body manages pressure. When an abscess drains, either naturally or through reduced inflammation, symptoms can lessen quickly. The sensation of relief is real, but it represents a shift in pressure, not necessarily the end of the infection. This is why a dental abscess is often remembered as something that comes and goes.
Culturally, many people also associate infections with visible signs. Once redness or swelling is no longer obvious, attention moves elsewhere. The quiet phase of a dental abscess can therefore feel misleadingly final.
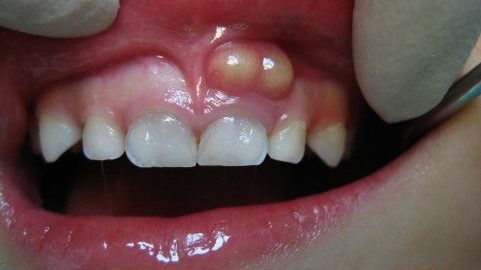
The role of time and the immune response in a dental abscess
Time plays an interesting role in how a dental abscess is perceived. The immune system is constantly active, attempting to contain and neutralize bacteria. In some cases, this response limits outward symptoms for extended periods.
This does not mean the infection has vanished. Instead, the immune system may be holding it in check. The abscess can remain dormant, with bacteria surviving in low activity states. This explains why a dental abscess may resurface weeks or even months later, often unexpectedly.
From a biological standpoint, this ongoing standoff between bacteria and immunity adds to the uncertainty. The absence of symptoms feels like healing, but the underlying dynamics may still be unfolding.
Common misconceptions surrounding a dental abscess
One widespread misconception is that antibiotics alone make a dental abscess disappear. While they can reduce bacterial load and inflammation, they do not always address the structural cause, such as damaged pulp or trapped infection pathways.
Another assumption is that draining pus solves the problem entirely. Drainage reduces pressure and discomfort, which is why it feels effective. However, without addressing the source, the environment that allowed the dental abscess to form may remain unchanged.
There is also a belief that small abscesses are harmless. Size does not always reflect activity. A small dental abscess can still involve complex bacterial behavior beneath the surface.
Why recurrence shapes the story of a dental abscess
Recurrence is a major reason why the topic of a dental abscess generates so many questions. When symptoms return after a quiet period, it challenges the idea of resolution. This cycle creates frustration and curiosity.
From a narrative perspective, recurrence turns a single event into an ongoing story. People begin to track patterns, triggers, and sensations. The dental abscess becomes something remembered over time rather than a one time episode.
This repeating pattern also influences how people talk about the condition. It is often described in phases rather than a clear beginning and end, reinforcing the sense that it behaves unpredictably.
How perception influences understanding of a dental abscess
Perception shapes memory. If the most intense pain fades, that relief dominates recollection. The quieter biological processes happening underneath are less noticeable and therefore less memorable.
This selective memory explains why many descriptions of a dental abscess focus on pain rather than cause. The mind prioritizes sensation over structure. As a result, understanding remains incomplete even when experience feels vivid.
Language also plays a role. Words like infection and abscess suggest something temporary. This framing influences how people interpret improvement, even when complexity remains.
The long view of what it means for a dental abscess to go away
In a broader sense, asking how a dental abscess goes away is really asking how the body resolves imbalance. It is not always a single moment of healing, but a gradual shift in conditions.
Some abscesses remain stable for long periods. Others change quickly. This variability makes universal answers difficult and fuels ongoing discussion. The story of a dental abscess is shaped by biology, perception, and time working together.
Rather than a clear finish line, the experience often feels like a series of chapters. That layered nature is why the question continues to resonate. A dental abscess is not just an infection. It is a process that unfolds, pauses, and sometimes returns, leaving people curious about where it truly ends.