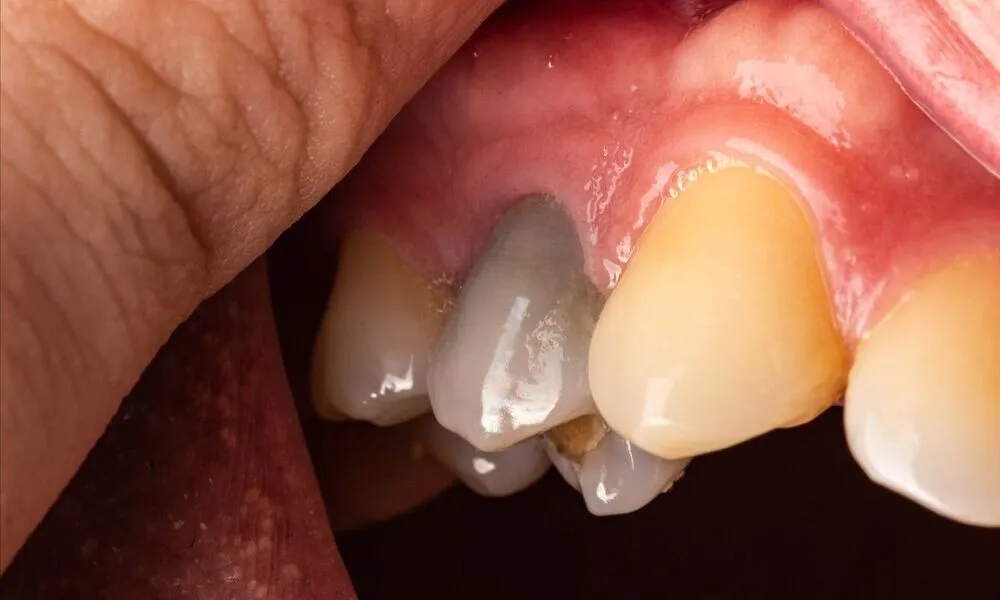
A dead tooth can sneak up silently, often without immediate pain, leaving many to wonder if it’s salvageable or destined for extraction. Understanding what causes a tooth to die, how to recognize the symptoms, and exploring prevention strategies can make the difference between losing a tooth and saving it.
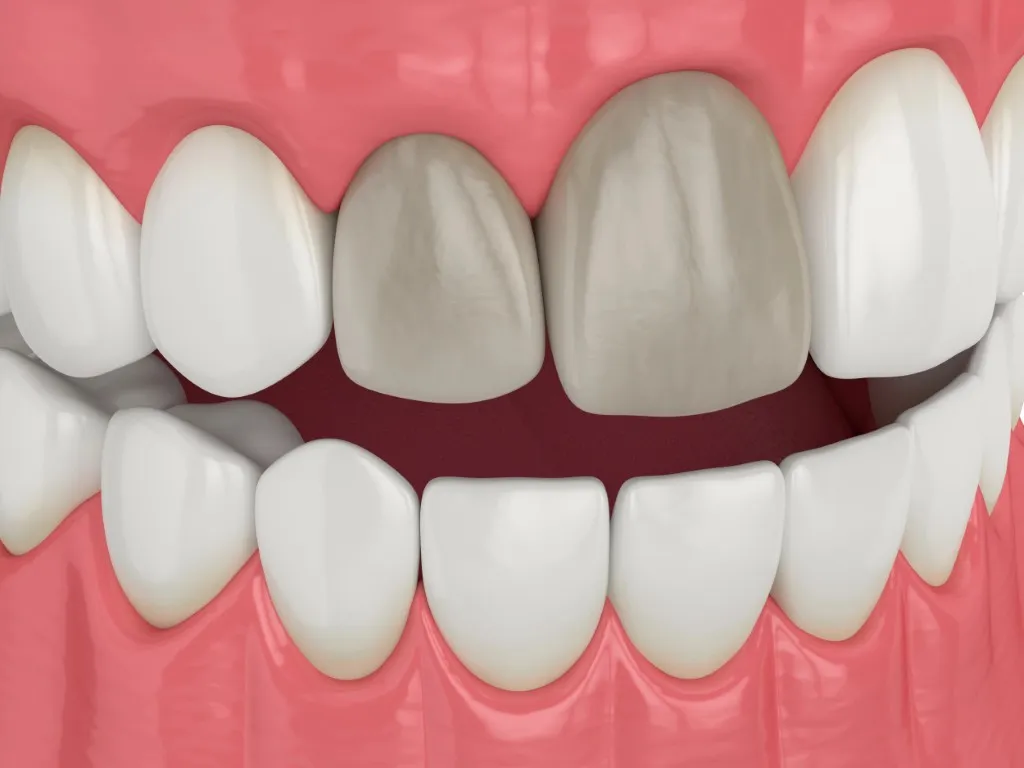
What Exactly Is a Dead Tooth?
A dead tooth, also referred to as a non-vital tooth, occurs when the pulp the innermost part containing nerves and blood vessels loses its vitality. The pulp can die due to trauma, untreated decay, or prolonged infections. Interestingly, a tooth can remain structurally intact while being non-vital, which is why early detection is crucial.
The pulp’s death triggers a chain reaction. Without blood flow, the tooth can no longer receive nutrients, making it more susceptible to fractures and bacterial invasion. Some studies suggest that even asymptomatic teeth can harbor infections that silently affect overall oral health.
Causes of a Dead Tooth
- Trauma or Injury: A sudden blow or accident can damage blood vessels, cutting off the tooth’s nourishment.
- Untreated Decay: Deep cavities can reach the pulp, causing irreversible damage.
- Severe Gum Disease: Periodontal infections can extend to the pulp, leading to necrosis.
- Repeated Dental Procedures: Multiple treatments on a tooth may stress the pulp and eventually lead to death.
Each cause has distinct mechanisms, but the outcome is the same: the pulp loses function, leaving the tooth non-vital.
Recognizing Symptoms of a Dead Tooth
A dead tooth does not always hurt, which makes it challenging to identify without a dental examination. However, there are common signs that indicate a tooth might be non-vital:
- Darkening of the tooth compared to surrounding teeth
- Sensitivity to temperature changes or pressure
- Swelling in the gums around the tooth
- Occasional throbbing pain, especially if infection develops
Interestingly, some teeth remain asymptomatic for years. Research in endodontics indicates that reliance solely on symptoms can be misleading; periodic dental check-ups are essential for early detection.
Can You Save a Dead Tooth?
The short answer: sometimes. Saving a dead tooth depends on the extent of pulp damage and the presence of infection. Endodontic procedures like root canal therapy are designed to clean out the dead pulp, disinfect the canals, and restore the tooth’s function.
Factors influencing success include:
- Timeliness of intervention
- Tooth location and structure
- Extent of bacterial invasion
Table: Comparison of Intervention Options for a Dead Tooth
| Treatment Option | Description | Success Rate | Ideal For |
| Root Canal Therapy | Removal of dead pulp, sealing canals | 85–95% | Most teeth with non-vital pulp |
| Dental Crown Post-Procedure | Adds structural support | 90% | Weakened teeth post-root canal |
| Extraction | Complete removal | N/A | Severely damaged or infected teeth |
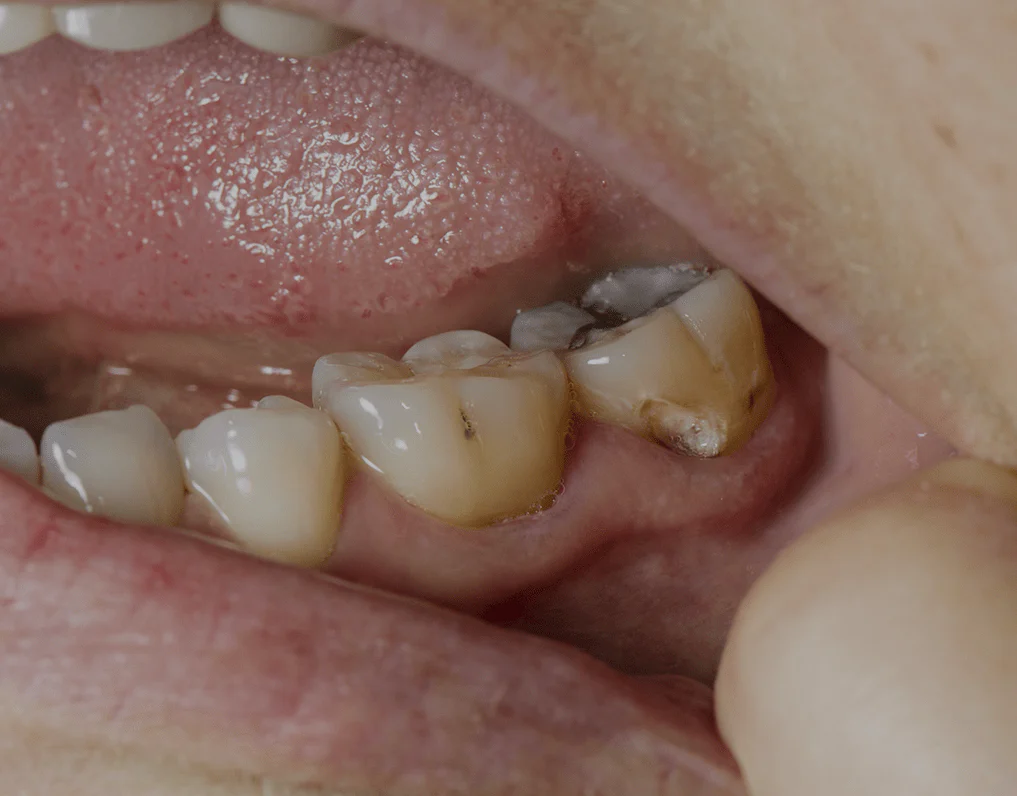
Prevention Strategies for Dead Tooth Formation
While accidents happen, several measures can minimize the risk of developing a dead tooth:
- Regular Dental Check-ups: Early detection of decay or trauma can prevent pulp death.
- Good Oral Hygiene: Brushing, flossing, and fluoride use reduce bacterial threats to the pulp.
- Protective Gear: Mouthguards in contact sports reduce trauma risk.
- Timely Treatment of Cavities: Prevents decay from reaching the pulp.
Scientific evidence suggests that a combination of preventive care and early intervention dramatically improves the odds of retaining natural teeth.
The Role of Diet and Lifestyle in Tooth Vitality
Diet plays a surprising role in maintaining tooth vitality. Nutrients such as calcium, vitamin D, and phosphates support the structural integrity of enamel, indirectly protecting the pulp from bacterial invasion. Limiting sugary foods reduces decay risk, which is a leading cause of pulp death. Studies have also linked smoking and alcohol consumption to impaired oral circulation, potentially contributing to pulp necrosis.
When a Dead Tooth Becomes Dangerous
Left untreated, a dead tooth can harbor bacteria, leading to abscess formation or systemic health issues. Symptoms indicating urgency include persistent pain, swelling, and discharge near the tooth root. Research highlights that even seemingly minor non-vital teeth can contribute to inflammatory conditions elsewhere in the body, emphasizing the importance of monitoring and timely care.
Innovative Approaches in Saving Dead Teeth
Recent advances in endodontics, including regenerative procedures, aim to revitalize or replace lost pulp tissue. Techniques using stem cells or bioactive scaffolds are being explored in clinical trials to restore pulp vitality, especially in younger patients. Although these approaches are not yet mainstream, they represent a promising frontier for preserving natural dentition.
A dead tooth does not always mean inevitable loss. Awareness of causes, symptom recognition, and timely dental intervention can make a significant difference. Preventive strategies, proper hygiene, and innovative treatment options are crucial in maintaining oral health and preserving natural teeth. Understanding the life cycle of a tooth from vitality to potential necrosis empowers patients to make informed decisions and engage proactively with their dental care.