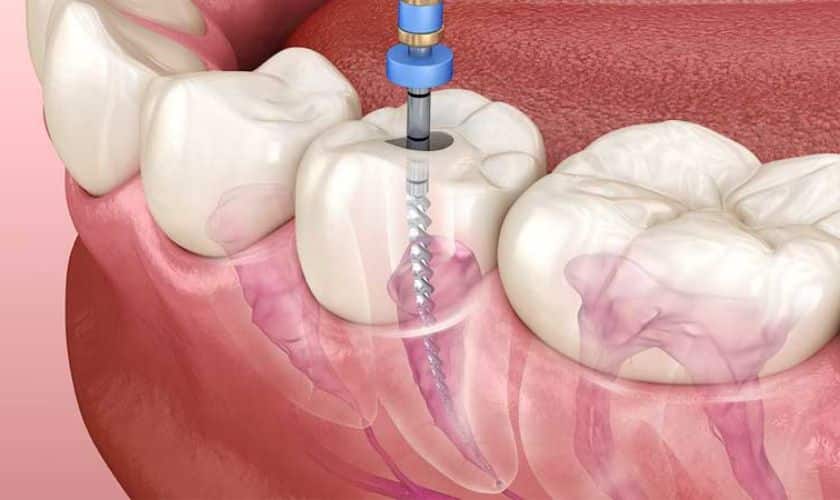
Root Canal Treatment is a cornerstone of modern dentistry, designed to save teeth affected by deep decay or infection. However, not all procedures achieve long-term success. Understanding the signs of failed Root Canal Treatment is crucial for patients, dentists, and researchers who want to assess treatment outcomes accurately. Failure does not always mean immediate pain; subtle indicators can hint at complications that may compromise oral health over time.
In this article, we explore the technical, clinical, and psychological aspects of Root Canal Treatment failures, providing a comprehensive guide that balances scientific insight with accessible explanations.
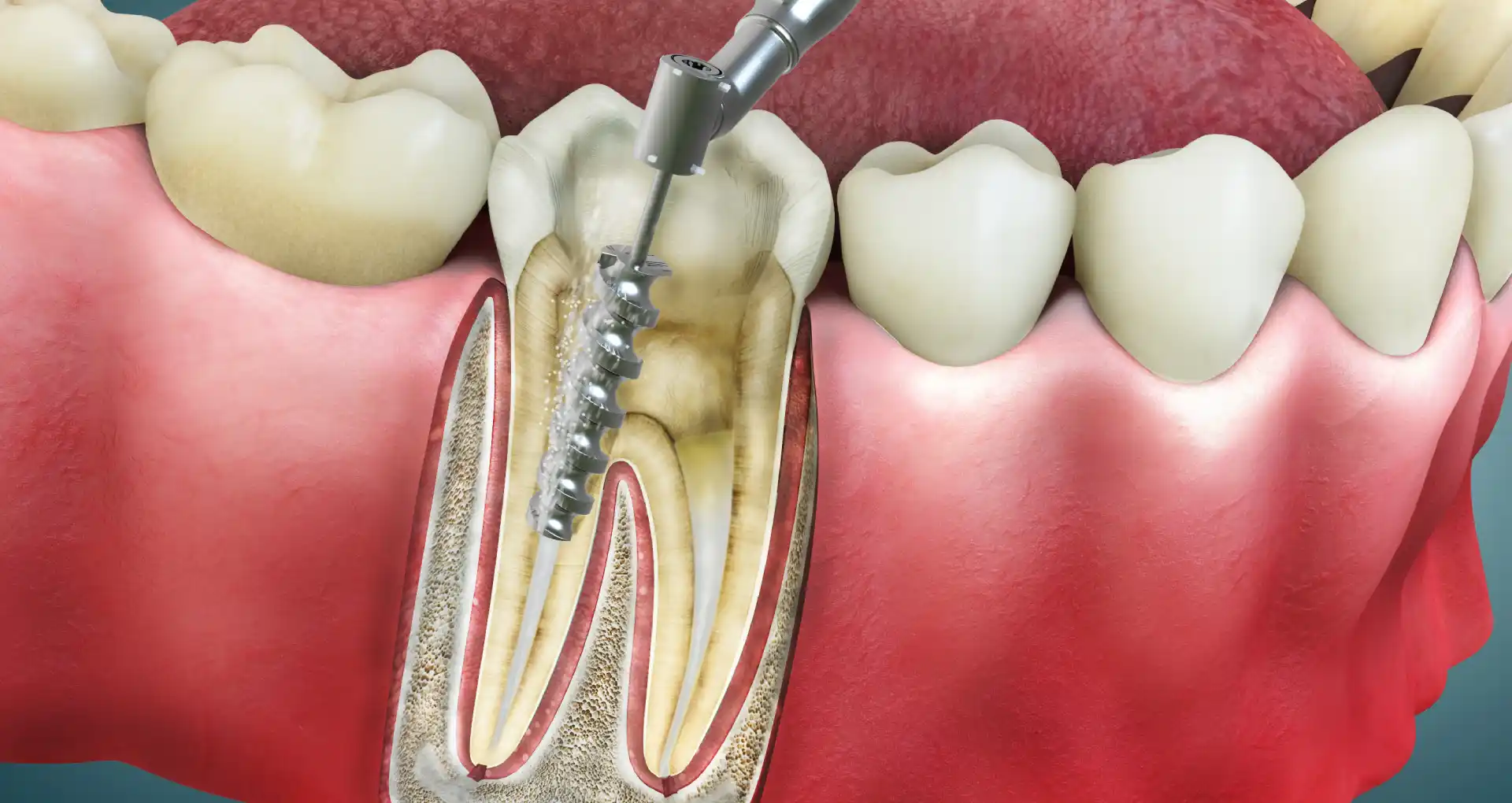
Historical Context of Root Canal Treatment Success and Failure
The evolution of Root Canal Treatment dates back over a century, with innovations in instrumentation, irrigation solutions, and filling materials. Early techniques had higher failure rates due to limited visibility, rudimentary sterilization methods, and less effective sealing materials. Today, advancements in microscopic endodontics and biocompatible sealers have significantly improved outcomes.
However, even with state-of-the-art technology, historical data shows that failure rates range between 5% and 15% depending on tooth type, initial infection severity, and operator expertise. Understanding this context helps patients interpret what a failed Root Canal Treatment truly represents a complication influenced by multiple factors rather than a simple procedural error.
Common Clinical Signs of Failed Root Canal Treatment
Patients often notice subtle changes in oral health that may indicate a failed Root Canal Treatment. Persistent or recurring pain, sensitivity to hot or cold, swelling of the gums, and discomfort when biting are key signals. These symptoms can emerge weeks, months, or even years after the procedure.
Clinical evaluations usually include radiographic imaging, which may reveal periapical lesions, missed canals, or incomplete filling. Sometimes, patients remain asymptomatic, highlighting the importance of regular dental check-ups. Observing these signs early allows for timely intervention, reducing the risk of further complications such as abscess formation or tooth loss.
Technical Causes Behind Root Canal Treatment Failures
Not all failures are caused by patient factors. Many originate from technical challenges during the procedure. Complex root anatomy, calcified canals, or undetected accessory canals can prevent complete cleaning and filling. In addition, microleakage caused by suboptimal sealing materials or restorative delays can lead to bacterial reinfection.
Instrumentation technique also plays a role. Using incorrect files, excessive force, or improper irrigation protocols can damage the canal system, increasing the likelihood of post-treatment complications. These technical nuances underscore why even minor deviations during Root Canal Treatment can have long-term effects on success.
The Role of Microbial Contamination
One of the most critical factors in Root Canal Treatment outcomes is microbial presence. Bacteria remaining inside untreated canals, dentinal tubules, or accessory branches can trigger reinfection. Biofilm formation within the root system further complicates treatment, making eradication challenging even with contemporary disinfection methods.
Studies show that teeth with persistent apical periodontitis often harbor specific bacterial strains resistant to conventional irrigants. Recognizing the microbial dimension explains why some Root Canal Treatments fail despite apparently perfect procedures, and why retreatment or surgical interventions are sometimes necessary.
Non-Surgical Interventions After Failure
When signs of a failed Root Canal Treatment are detected early, conservative options may suffice. Retreatment involves removing old filling materials, re-cleaning the canals, and re-sealing them. Modern techniques using magnification and ultrasonic instruments improve the chances of success compared to initial attempts.
In addition, adjunctive therapies such as antimicrobial irrigation, temporary medicaments, or enhanced obturation materials can improve outcomes. Patients who adhere to post-operative care, including oral hygiene and routine monitoring, often experience better recovery and reduced recurrence of infection.
Surgical Approaches for Persistent Root Canal Treatment Failure
Despite the best non-surgical interventions, some Root Canal Treatment failures persist due to complex anatomy or resistant infections. In such cases, surgical procedures like apicoectomy or intentional replantation may be necessary. An apicoectomy involves removing the tip of the tooth root and sealing the canal from the end, eliminating residual infection that standard retreatment cannot reach.
Surgical interventions are precise and require thorough imaging and planning. While more invasive than retreatment, these procedures often save teeth that would otherwise need extraction, preserving function and aesthetics. Understanding surgical solutions helps patients appreciate the range of options available when conventional Root Canal Treatment fails.
Impact of Patient Factors on Root Canal Treatment Success
The success of Root Canal Treatment is not solely dependent on the dentist’s skill. Patient-specific factors such as age, systemic health, immune response, and oral hygiene play a pivotal role. For example, diabetes or immunocompromised conditions may reduce healing efficiency, increasing the likelihood of treatment failure.
Behavioral factors, including bruxism, irregular dental check-ups, or delayed restorative care, can exacerbate complications. Recognizing these influences allows both clinicians and patients to adopt proactive strategies, improving the prognosis of Root Canal Treatment outcomes.
The Psychological and Behavioral Dimension of Root Canal Treatment Failure
Failed Root Canal Treatment can carry psychological consequences. Chronic pain, repeated dental visits, or prolonged recovery may increase anxiety around oral care. This often results in delayed treatment, perpetuating a cycle of discomfort and fear.
Behavioral strategies, such as guided dental education and patient counseling, can mitigate these effects. Understanding the psychological dimension emphasizes that dental health is not only a mechanical or microbial issue it intertwines with patient experience and emotional well-being.
Radiographic and Imaging Evaluation of Failed Root Canal Treatment
Modern dentistry relies heavily on imaging to assess Root Canal Treatment success. Periapical X-rays, cone-beam computed tomography (CBCT), and digital imaging provide detailed views of the root canal system. These tools help identify missed canals, micro-fractures, or persistent lesions.
Accurate interpretation of imaging data enables dentists to tailor retreatment or surgical plans. By comparing pre-treatment and post-treatment images, clinicians can gauge the effectiveness of previous procedures and anticipate potential complications, ensuring informed decision-making in ongoing care.
Consequences of Untreated Root Canal Treatment Failure
Ignoring a failed Root Canal Treatment can lead to serious oral and systemic complications. Persistent infection may cause abscess formation, bone loss, and eventual tooth loss. In rare cases, untreated infections can spread, affecting surrounding tissues or entering systemic circulation, which highlights the critical importance of timely intervention.
Long-term untreated failures can also impact aesthetics and chewing efficiency. Teeth with compromised structural integrity may fracture or become increasingly difficult to restore. Recognizing the potential consequences underscores the need for monitoring and proactive management.
Role of Restorative Materials in Maintaining Root Canal Treatment Success
Even after technically successful Root Canal Treatment, the choice of restorative material is critical. Crowns, inlays, or onlays protect the tooth from fractures and prevent bacterial reinfection. Inadequate restorations can compromise the success of the treatment, emphasizing the importance of integrating endodontics with prosthetic planning.
Advanced materials, such as fiber-reinforced composites or ceramic crowns, offer both durability and aesthetic appeal. Ensuring proper fit and sealing further reduces the risk of secondary infection, highlighting the interplay between endodontics and restorative dentistry.
Preventive Measures and Long-Term Monitoring
Patients can actively contribute to the longevity of their Root Canal Treatment. Maintaining excellent oral hygiene, attending regular dental check-ups, and monitoring for unusual symptoms help prevent failures or detect them early.
Education about warning signs such as swelling, prolonged sensitivity, or unexplained discomfort empowers patients to seek timely care. Long-term follow-up, including periodic radiographic assessment, ensures that any complications are addressed before they escalate.
The Role of Advanced Endodontic Technology
Recent innovations in Root Canal Treatment have significantly reduced failure rates. Microscopic endodontics, ultrasonic cleaning, and advanced irrigation systems improve canal debridement and disinfection. Biocompatible sealers and 3D imaging further enhance procedural precision.
These technologies allow clinicians to detect hidden anatomical complexities and ensure thorough cleaning, reducing microbial persistence. Patients benefit from improved outcomes and fewer retreatments, emphasizing the importance of technology in modern endodontics.
Integrating Multidisciplinary Approaches in Root Canal Treatment Failure
Failed Root Canal Treatment often requires collaboration between endodontists, restorative dentists, and sometimes oral surgeons. This multidisciplinary approach ensures comprehensive evaluation and maximizes the chances of saving the tooth. Each specialist contributes unique expertise: endodontists focus on canal debridement, restorative dentists optimize structural integrity, and surgeons address anatomical challenges surgically.
Collaboration also enables personalized treatment plans. For example, a tooth with complex canal anatomy may first undergo retreatment under a microscope, followed by a precision crown placement to prevent future complications. Integrating multiple disciplines ensures that patients benefit from the full spectrum of modern dental care when facing Root Canal Treatment failure.
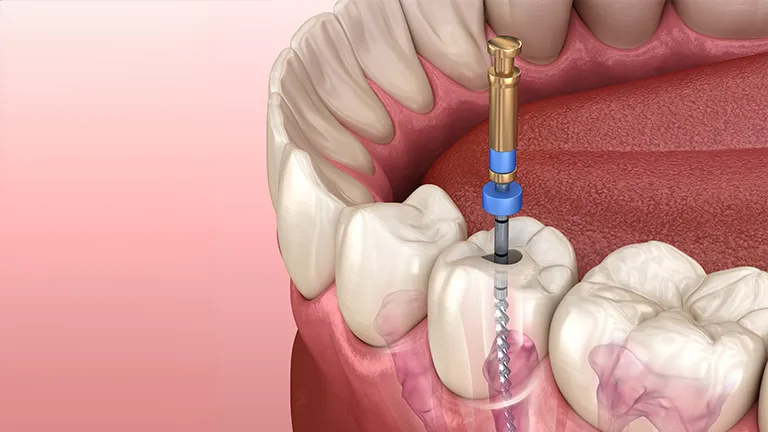
Advanced Retreatment Techniques
When initial Root Canal Treatment fails, retreatment can address persistent infection. Modern retreatment techniques use rotary instruments, ultrasonic activation, and enhanced irrigation protocols to remove previous filling materials and disinfect the canal thoroughly.
Retreatment is often preferred over extraction because it preserves natural tooth structure. Success depends on accurate diagnosis, proper cleaning, and sealing. Clinicians also use magnification and digital imaging to identify missed canals or micro-fractures that could contribute to failure, highlighting the precision required in modern endodontics.
Impact of Oral Microbiome on Root Canal Treatment Failure
The oral microbiome plays a critical role in the success of Root Canal Treatment. Certain bacterial strains, such as Enterococcus faecalis, are notoriously resilient and can survive standard cleaning procedures, leading to persistent infection.
Understanding microbial dynamics allows dentists to tailor irrigation solutions and medicaments to target resistant bacteria. Ongoing research explores probiotics and antimicrobial strategies that may enhance long-term outcomes. Awareness of microbiological factors underscores that endodontic success is not solely mechanical but also biological.
Signs and Symptoms of Failed Root Canal Treatment
Identifying failed Root Canal Treatment involves recognizing clinical symptoms. Common indicators include persistent pain, swelling, sensitivity to pressure or temperature, and discoloration of the tooth. Chronic infection may also produce gum abscesses or fistulas.
Timely recognition of these signs allows for early intervention, preventing more severe complications. Patients should be educated to monitor for subtle changes, as early detection dramatically improves prognosis and reduces the need for invasive procedures.
Long-Term Prognosis and Patient Education
Understanding the long-term outlook after Root Canal Treatment is essential for patient decision-making. Teeth that are properly retreated, restored, and monitored can last decades, while untreated failures often result in extraction.
Patient education is key to preserving treatment outcomes. Emphasizing oral hygiene, regular follow-ups, and adherence to recommended restorative care ensures that the tooth remains functional and healthy. A well-informed patient actively participates in safeguarding the success of their endodontic therapy.
Consequences of Ignoring Failed Root Canal Treatment
Failure to address a compromised Root Canal Treatment can lead to a cascade of issues: spreading infection, jawbone deterioration, sinus involvement in upper teeth, and systemic health risks in severe cases. Additionally, prolonged infection can increase discomfort and reduce quality of life.
Proactive management mitigates these consequences, underscoring the importance of recognizing failure early and choosing appropriate interventions. Patients benefit from understanding both the medical and functional implications of untreated endodontic complications.
The Future of Root Canal Treatment and Failure Management
Emerging technologies in endodontics, including AI-guided imaging, laser-assisted disinfection, and bioactive sealers, promise to reduce failure rates further. These innovations allow more accurate canal mapping, improved bacterial eradication, and better long-term outcomes.
As dental science evolves, patients can expect more precise, less invasive, and longer-lasting solutions for managing failed Root Canal Treatment. Awareness of these advancements provides insight into how the field continues to address challenges while enhancing patient care.
Final Reflections on Root Canal Treatment Failure
Failed Root Canal Treatment is a complex issue involving anatomical, microbial, technical, and behavioral factors. Understanding these dimensions allows clinicians to craft comprehensive treatment strategies and patients to make informed decisions.
By recognizing early signs, leveraging advanced techniques, and integrating multidisciplinary approaches, the consequences of treatment failure can be minimized. Ultimately, this topic highlights the interplay between clinical expertise, patient involvement, and technological innovation in modern dentistry.