Healthy gums rarely ask for attention. They sit quietly around the teeth, doing a difficult job with almost no applause. But Gum Inflammation changes that silence. It can begin with a trace of redness, a little puffiness, or bleeding during brushing, then slowly turn everyday oral care into a source of discomfort and concern. At Livera Clinic, this topic matters because gum health is closely linked not only to the appearance of the smile, but also to comfort, confidence, and long-term oral function.
What makes this issue especially interesting is how ordinary it can seem at first. Many people notice irritated gums and assume they brushed too hard or ate something sharp. Sometimes that may be true. Yet in many cases, swollen or inflamed gum tissue reflects a more complex process involving bacteria, plaque accumulation, immune response, lifestyle habits, and general health patterns. In other words, the gums are not simply “angry”; they are reacting to conditions that deserve careful attention.
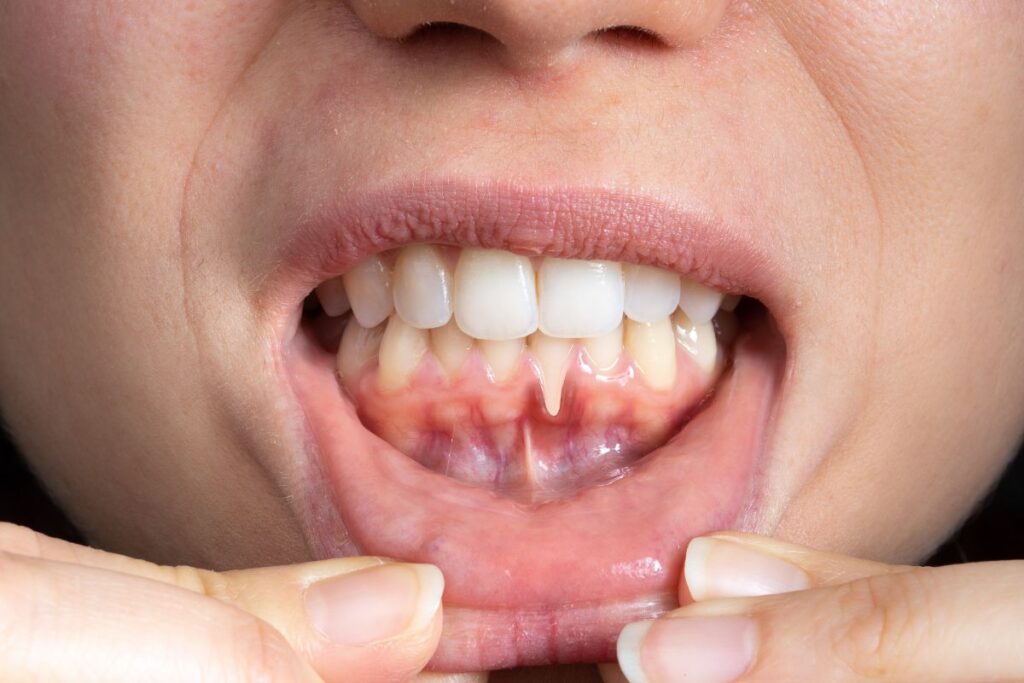
What Is Gum Inflammation and Why Does It Happen?
Gum Inflammation generally refers to the body’s response to irritation or harmful buildup affecting the gingival tissues. In many situations, this process begins when plaque a sticky biofilm rich in bacteria collects along the gumline. If not removed effectively, that plaque may trigger an immune reaction. Blood flow increases, tissues swell, and the gums may become tender or prone to bleeding.
This response is not random. The mouth contains a complex microbial ecosystem, and the gums exist in constant interaction with that environment. When the balance shifts, the tissue may react defensively. Research over the years has shown that inflammation is not caused by “dirt” alone, but by a dynamic relationship between bacterial communities and the host immune system. Some people may experience mild gingival irritation for a short time, while others may develop more persistent periodontal inflammation.
A range of factors may contribute to inflamed gums. Poor oral hygiene is often central, but it is rarely the whole story. Smoking, hormonal fluctuations, stress, certain medications, dry mouth, orthodontic appliances, diabetes, and nutritional imbalances may all influence how gum tissue responds. Even mouth breathing and clenching habits can make tissues more vulnerable. That is why Gum Inflammation should be understood as a condition with multiple layers rather than a one-cause problem.
Another important point is that the gums do not always signal trouble with dramatic pain. Unlike a toothache, gum irritation can be deceptively quiet. A person may continue with daily life while the inflammatory process develops slowly over weeks or months. This low-noise pattern is one reason gum disease has such a wide global prevalence.
Common Gum Inflammation Symptoms People Often Notice Late
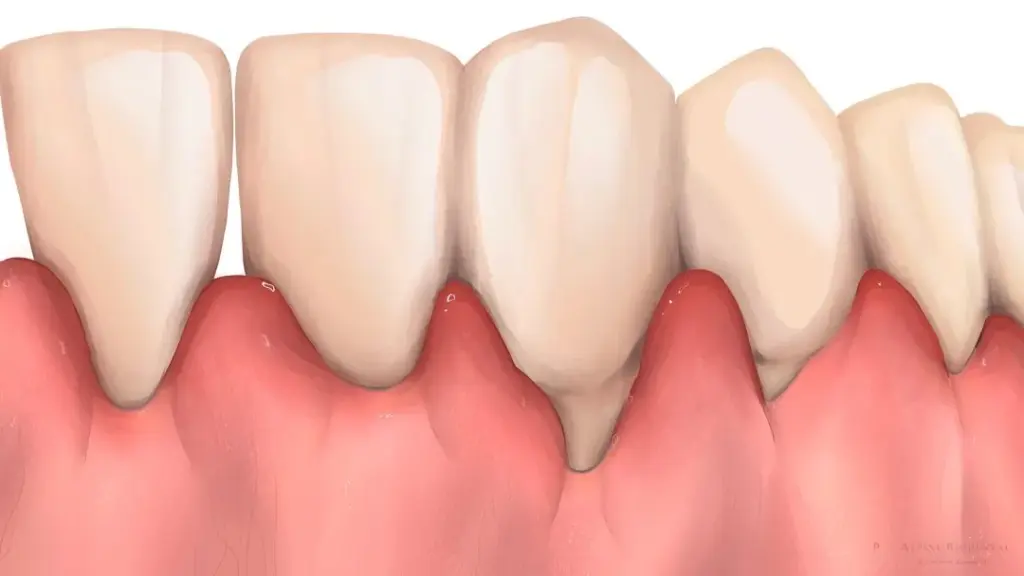
One of the most recognizable signs of Gum Inflammation is bleeding during brushing or flossing. Many people dismiss this as normal, but healthy gums usually do not bleed easily. Bleeding may appear alongside redness, swelling, or a glossy surface instead of the firm, pale pink texture associated with healthier gingiva.
Another frequent symptom is tenderness. The gums may feel sore when eating crunchy foods or when touched by a toothbrush. In some cases, they may recede slightly, making teeth look longer than before. Others notice persistent bad breath, an unpleasant taste, or a sensation that the gums feel “full” or irritated. These changes may seem small individually, but together they can suggest active soft tissue inflammation.
Below is a simple overview of symptoms often associated with gum irritation and periodontal inflammation:
| Symptom | What It May Look or Feel Like | Why It Matters |
| Bleeding gums | Blood during brushing or flossing | Often an early sign of gingival inflammation |
| Redness | Gums appear darker or brighter red than usual | Suggests increased blood flow and irritation |
| Swelling | Puffy gum margins | May indicate immune response to plaque or irritation |
| Tenderness | Pain or soreness when cleaning teeth | Can affect oral hygiene quality |
| Bad breath | Ongoing unpleasant breath odor | Sometimes linked to bacterial buildup |
| Gum recession | Teeth look longer | May reflect tissue changes over time |
Symptoms do not always appear in the same combination. Some people experience visible swelling without pain. Others notice bad breath before they notice bleeding. Because Gum Inflammation can be subtle, it often progresses further than expected before it receives proper attention.
It is also worth noting that symptom intensity does not always match severity. A person with only mild discomfort may still have meaningful tissue changes, while another with obvious sensitivity may have a more limited problem. That is one reason self-interpretation can be unreliable.
Gum Inflammation Causes Beyond Poor Brushing Habits
It is tempting to reduce Gum Inflammation to a hygiene issue, but that explanation is too narrow. Plaque is a key factor, yet the gum tissues are influenced by broader biological and behavioral conditions. For example, smoking has long been associated with altered blood flow, impaired healing patterns, and changes in immune response. Interestingly, smokers may show less obvious bleeding even when gum disease is present, which can make the condition easier to overlook.
Hormonal changes may also affect gum tissue behavior. Pregnancy, puberty, menopause, and menstrual cycle variations are all associated in some individuals with greater gum sensitivity. This does not mean hormones “cause” gum disease in a simple way, but they may change the tissue response to plaque and bacterial load. Similarly, medications that reduce saliva or alter gum tissue volume can create an environment in which inflammation becomes more likely.
Systemic health may play a role as well. Researchers have examined links between periodontal conditions and diabetes, cardiovascular health markers, and chronic inflammatory burden. While these relationships are complex and still discussed in nuanced ways, the mouth is increasingly understood as part of a larger physiological network. Inflamed gums are not isolated from the rest of the body’s processes.
Diet and daily routine can further shape the environment. Frequent sugar exposure may support bacterial activity, while chronic stress may affect immune regulation and hygiene habits at the same time. Sleep quality, hydration, and oral breathing patterns can all subtly influence the oral ecosystem. In many cases, Gum Inflammation develops through the accumulation of several small factors rather than one dramatic trigger.
From Gingivitis to Deeper Problems: How Gum Inflammation Can Progress
In its earlier stage, Gum Inflammation is often described as gingivitis. This usually means inflammation is limited to the gum tissue without deeper attachment loss around the teeth. Gingivitis may be reversible in many cases when the irritants are managed effectively. That makes early recognition especially important.
If inflammation persists over time, however, the situation may become more complex. The tissues supporting the teeth include not only gums, but also bone and connective structures. When the inflammatory process moves deeper and begins to affect these supporting tissues, the condition may fall into the broader category of periodontal disease. At this stage, pockets may form between the teeth and gums, making plaque control more difficult and allowing bacterial communities to persist.
This progression is not inevitable for every person with irritated gums. Some individuals may remain at a mild inflammatory stage, while others may be more susceptible to tissue breakdown because of genetic tendencies, systemic conditions, or long-term environmental exposure. The science here is especially fascinating: periodontal disease is not simply a bacterial attack, but a host-mediated inflammatory process in which the body’s own response contributes to tissue damage.
Understanding progression matters because Gum Inflammation is often easier to manage before structural support is affected. Once attachment or bone changes occur, treatment may become more involved and long-term monitoring more important. This is one reason dental professionals often pay close attention to bleeding, pocket depth, plaque retention areas, and tissue contour during examination.

How Gum Inflammation Is Usually Evaluated in Dental Settings
A proper evaluation of Gum Inflammation usually starts with observation. The color, texture, contour, and firmness of the gums can reveal a great deal. Healthy gums often appear firm and shaped neatly around the teeth, while inflamed gums may look swollen, smooth, or shiny. Bleeding on gentle probing is another sign frequently considered in clinical assessment.
Dental professionals may also examine plaque accumulation, tartar deposits, gum pocket depth, and any signs of recession. In some cases, radiographs may be used to check whether there are changes involving supporting bone. This matters because visible redness alone does not fully explain what is happening underneath the gumline. A more complete periodontal evaluation helps distinguish temporary irritation from a more established disease pattern.
Assessment is not only about identifying damage. It is also about understanding contributing conditions. A clinician may consider oral hygiene routines, smoking history, medication use, orthodontic appliances, dry mouth, medical background, and even the location of inflammation. For instance, localized swelling around one tooth may suggest a different scenario from generalized gingival redness across the whole mouth.
Because Gum Inflammation has many possible influences, the most useful evaluations are often both visual and contextual. The same symptom may mean different things depending on the patient’s habits, anatomy, and oral history. That is why a careful assessment often provides more clarity than assumptions based on internet images or temporary sensations.
Gum Inflammation Treatments Commonly Considered
When discussing Gum Inflammation, treatment usually depends on the cause, severity, and whether deeper periodontal structures are involved. In many cases, the first approach centers on reducing plaque and bacterial accumulation. Professional cleaning may help remove tartar and deposits that cannot be addressed through home brushing alone. If the issue remains limited to gingival inflammation, improving oral hygiene efficiency may significantly change the tissue response over time.
When deeper pockets or more advanced periodontal changes are present, treatment may become more structured. Dental professionals may consider non-surgical periodontal therapy aimed at cleaning beneath the gumline and disrupting bacterial biofilm in areas that are difficult to access. The exact method varies, and outcomes depend on many factors, including patient adherence, anatomy, smoking status, and baseline tissue condition.
Below is a general outline of approaches often associated with inflamed gum management:
- Clinical examination and periodontal assessment
- Professional plaque and tartar removal
- Review of brushing and interdental cleaning technique
- Monitoring of bleeding, swelling, and pocket changes
- Re-evaluation to assess tissue response
- Further periodontal care if deeper involvement is suspected
Some situations may also involve discussion of mouth rinses, local antimicrobial support, restoration adjustments, or management of plaque-retentive dental work. In more advanced cases, surgical periodontal procedures may be part of the broader conversation. It is important, however, to avoid viewing treatment as a one-time event. Gum Inflammation often behaves more like a condition that requires ongoing control rather than a single dramatic cure.
The good news is that gum tissues can respond remarkably well when irritants are reduced and maintenance improves. The less cheerful truth is that they can also relapse when the original conditions return. That push-and-pull nature makes long-term consistency more important than quick fixes.
Daily Patterns That May Influence Gum Inflammation Recurrence
One of the more frustrating things about Gum Inflammation is its tendency to return. A person may notice improvement after cleaning or more attentive brushing, then see bleeding come back weeks later. This recurrence is not unusual. Plaque biofilm rebuilds quickly, and gum tissues respond to repeated irritation with surprising consistency.
Technique matters just as much as frequency. Brushing twice a day sounds excellent on paper, but if plaque remains concentrated near the gumline or between the teeth, inflammation may persist. Interdental cleaning is often overlooked for this reason. The spaces between teeth are prime real estate for bacteria, and standard brushing may not address them effectively. Appliances, crowding, and restorations can make those areas even more difficult to manage.
Lifestyle can also shape recurrence. Smoking, stress, irregular routines, dehydration, and high sugar snacking patterns may all contribute to an oral environment that favors persistent bacterial growth or impaired tissue recovery. Even highly motivated people can struggle if they use tools that do not suit their anatomy or if they have restorations that trap plaque.
This is why Gum Inflammation is best understood not as an isolated episode, but as a pattern that reflects the relationship between oral care, biology, and daily habits. The gums are excellent historians. They record what has been happening in the mouth, often with more honesty than a person’s memory of their hygiene routine.
Why Gum Inflammation Deserves More Attention Than It Gets
There is a tendency to rank oral health concerns by pain level. Tooth pain feels urgent; mild gum bleeding often does not. Yet Gum Inflammation deserves attention precisely because it can remain active without dramatic symptoms. It may affect comfort, appearance, breath quality, and long-term periodontal stability while remaining easy to ignore.
There is also a social dimension. Healthy-looking gums contribute to the aesthetics of a smile in a way people often notice subconsciously. Puffiness, redness, or recession can change the visual balance of the teeth and gums. In that sense, gingival health is not only clinical; it shapes facial expression, confidence, and the perceived freshness of the mouth.
From a scientific perspective, gum tissue is a fascinating interface between the immune system and a dense microbial environment. It is biologically active, highly vascular, and constantly adapting. Inflammation in this tissue is not trivial. It reflects a meaningful interaction between external biofilm and internal host response. That alone makes it worthy of more public understanding than it usually receives.
At Livera Clinic, the conversation around Gum Inflammation is best approached with clarity rather than alarm. Not every red gum signals severe disease, and not every bleeding point predicts serious loss. But the condition is important enough to be understood early, observed carefully, and discussed with nuance.
Gum Inflammation may begin quietly, but it is rarely meaningless. Whether it appears as bleeding during brushing, slight swelling, persistent bad breath, or visible redness, it often reflects a deeper conversation taking place between oral bacteria and the body’s immune system. That conversation can stay mild, or it can become more significant over time depending on habits, health conditions, and tissue response.
Understanding the symptoms and treatments of Gum Inflammation helps turn a vague concern into something more manageable and less mysterious. The topic sits at the crossroads of microbiology, daily hygiene, lifestyle, and periodontal science. It is common, often underestimated, and surprisingly informative about the state of oral health.
For readers trying to make sense of sore, swollen, or bleeding gums, the central idea is simple: gum tissue changes usually have a story behind them. The more clearly that story is understood, the easier it becomes to interpret what the mouth may be trying to say.