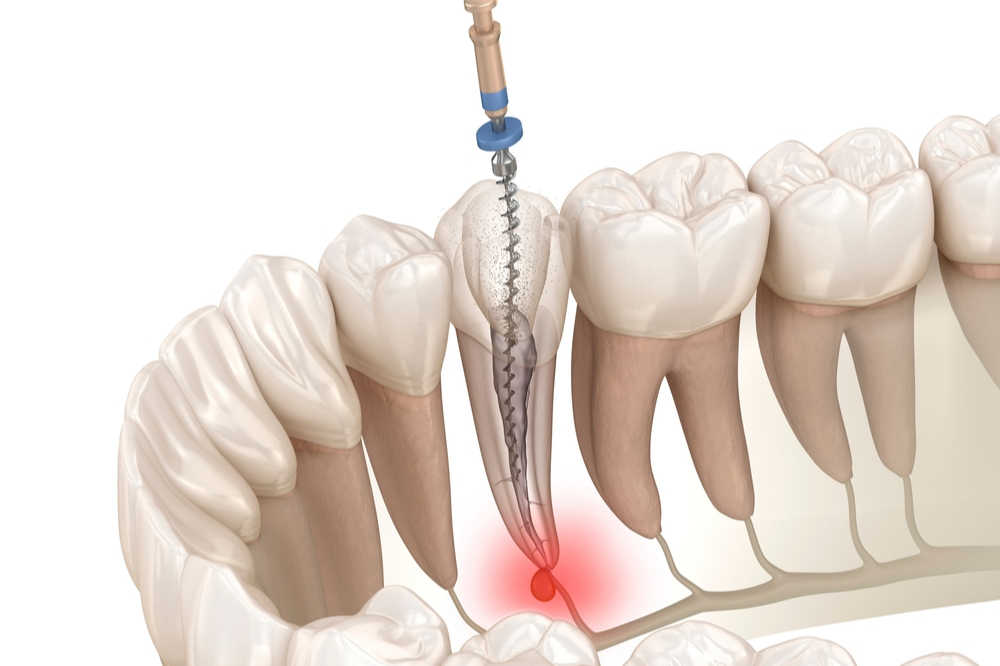
Understanding the complex structure of a dental nerve is one of the keys to making sense of why it sometimes becomes unresponsive, painful, or completely necrotic. When people hear the phrase nerve death, they often imagine a sudden collapse inside the tooth, but the process is usually gradual, influenced by chemical, mechanical, or bacterial factors. Because the dental nerve sits deep within the pulp chamber, it reacts to damage in ways that can be subtle at first and progressively more noticeable. This makes the topic both scientifically fascinating and emotionally relatable, especially for anyone who has ever felt that strange mixture of dull pressure and sharp sensitivity radiating from a single tooth.
Nerve necrosis inside a tooth has been studied for decades through biological models, patient case reports, and histological research. While none of these studies offer a universal rule for every individual, they do build a framework for understanding what might drive a tooth to lose vitality. In many situations, the process is tied to inflammation and the inability of the inner tissues to recover from stress. Because the dental nerve exists within a confined space, any swelling or bacterial invasion can quickly overwhelm it, eventually leading to the collapse of its functional cells. As complex as it sounds, the sequence is part biology, part environment, part lifestyle, and part genetics, which makes it a topic worth exploring layer by layer.
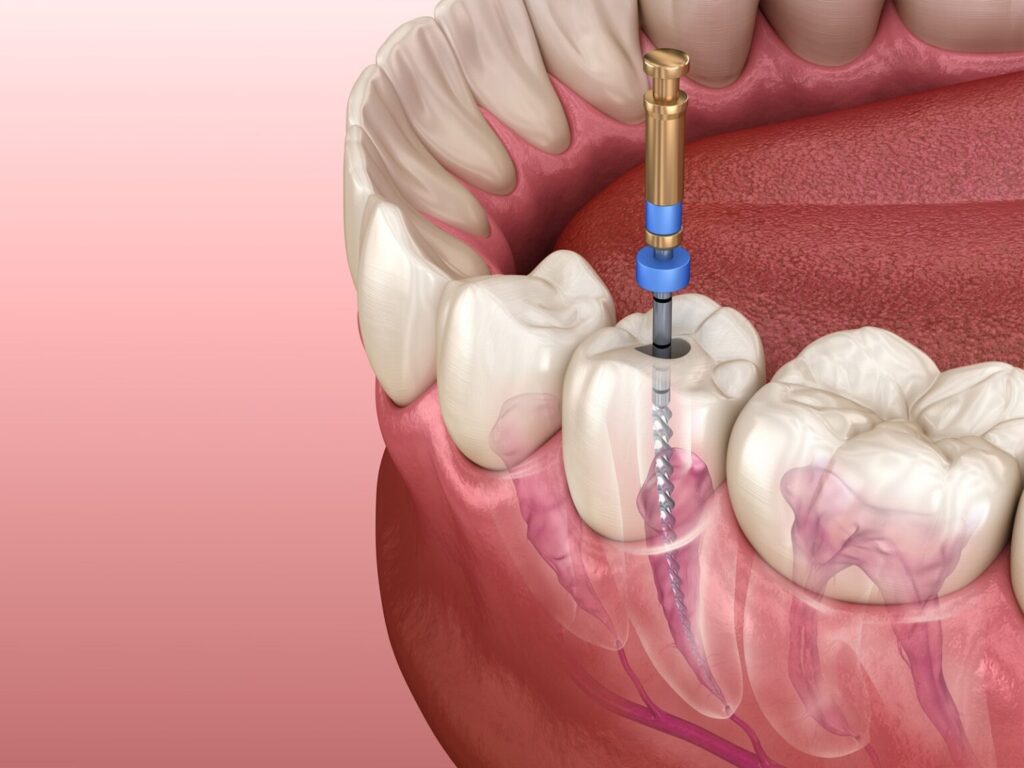
How the Dental Nerve Functions Inside a Living Tooth
To truly appreciate how nerve degeneration occurs, it’s valuable to understand how the system normally works. The dental nerve is not a single strand but a cluster of fibers responsible for sensing temperature, vibration, and pressure. They extend from deeper neural pathways and enter the tooth through narrow channels near the root. Although small in size, they are extremely important in keeping the tooth responsive and alive. In scientific descriptions, the nerve is referenced as part of the tooth’s “pulp complex,” a network containing blood vessels, connective tissues, and cellular structures.
Researchers often describe this system as one of the few body tissues that cannot expand during inflammation. Bones and skin allow swelling to distribute outward, but the pulp is restricted by rigid dentin walls. Because of this, once irritation becomes too intense, the dental nerve may not receive enough oxygen or nutrients. Scientific models show that even minor changes in internal pressure can lead to cellular fatigue. Over time, these small disturbances can contribute to reduced vitality, setting the stage for more severe degeneration.
Major Causes Behind Dental Nerve Degeneration
When people ask what triggers nerve death, the answer is rarely singular. Instead, it’s a combination of factors, each capable of disrupting the delicate balance inside the tooth. Trauma is one of the most studied causes. Even if a blow to the mouth does not visibly crack the enamel, the internal tissues can become bruised. The dental nerve may respond unpredictably, ranging from temporary sensitivity to complete shutdown weeks or even months later. This delayed reaction has been documented in various dental journals and remains one of the more surprising aspects of nerve behavior.
Another significant cause relates to deep tooth decay. Bacteria are remarkably adaptive and produce acids capable of penetrating enamel and dentin. Once they move closer to the pulp, they can create an inflammatory response that overwhelms the inner tissues. Studies indicate that bacterial biofilms near the pulp chamber drastically increase the risk of nerve necrosis. At the same time, repeated dental procedures on the same tooth can add mechanical stress. Grinding, polishing, drilling, and even heat from equipment may contribute to irritation. While modern techniques reduce these risks, they cannot eliminate them entirely, which keeps the dental nerve vulnerable in certain situations.
The Role of Inflammation in Nerve Death
Inflammation is at the center of nearly every discussion about nerve health inside a tooth. When triggered, the body sends cells to the irritated region in an attempt to restore balance. However, within the confined pulpal structure, this reaction becomes problematic. As pressure builds, the blood supply feeding the dental nerve can become restricted. Without proper circulation, the tissues struggle to maintain normal function.
Advanced imaging studies have shown that inflammatory markers within the pulp rise significantly in response to bacterial invasion or physical trauma. These markers contribute to swelling that has nowhere to go, compressing nerve fibers and eventually leading to reduced vitality. The longer this cycle continues, the higher the chance of irreversible damage. Because of this unique limitation, even mild inflammation inside the tooth can create long term consequences, particularly when left undetected.
Early Symptoms That Suggest Dental Nerve Decline
Many people are surprised to learn that nerve degeneration does not always begin with pain. In some cases, the earliest signs are subtle changes such as temperature sensitivity or a peculiar dull ache that comes and goes. These shifts can reflect changes in the internal pressure around the dental nerve . Some individuals describe the sensation as a cold wave spreading through the tooth, while others mention a lingering warmth after consuming hot beverages.
Additional signs may include discoloration, since the inner tissues influence the shade of the enamel above them. A tooth undergoing nerve decline might gradually darken or take on a grayish tone. Though not definitive, this can be a clue for further investigation. Another indicator is sensitivity to biting pressure. When the nerve begins to lose vitality, the surrounding tissues may react differently to force, creating an uncomfortable or unstable feeling. These symptoms do not confirm nerve death on their own, but they highlight the importance of understanding subtle shifts in tooth behavior.
How Trauma Disrupts the Dental Nerve System
Trauma is one of the most well known triggers for nerve injury inside a tooth, yet the internal process is far more complex than it appears on the surface. When a tooth receives a strong impact, the vascular channels inside the pulp may compress, limiting the normal flow of nutrients. This restricted circulation gradually affects the sensitivity and vitality of the inner tissues, sometimes causing the dental nerve to lose its natural responsiveness. What seems like a simple blow can therefore create a chain of microscopic events that unfold slowly.
For some individuals, trauma does not immediately show obvious signs. Sensitivity may temporarily heighten or diminish, only to stabilize later. This fluctuation often makes people think everything is normal, which is why nerve injury can remain unnoticed for long periods. The body attempts to compensate, but if the circulation inside the pulp chamber does not fully recover, the nerve may enter a progressive stage of deterioration. This gives trauma-related nerve changes a subtle but significant profile.
The Role of Microcirculation in Dental Nerve Health
The inner portion of a tooth relies on tiny blood vessels that branch like threads through the pulp chamber. These vessels are essential for delivering oxygen and nutrients to the nerve, regulating temperature responses, and maintaining normal sensitivity. When inflammation increases pressure inside this confined space, microcirculation becomes disrupted. Over time, this can slowly diminish the vitality of the dental nerve.
One interesting aspect is how the tooth reacts to limited circulation. Instead of shutting down immediately, the nerve often demonstrates periods of partial responsiveness. Many individuals notice occasional sensitivity to heat or cold without significant pain. These small sensory clues reflect early vascular stress within the pulp. While not definitive indicators of nerve death, they show how delicately the system functions.
Slow Progression: How Cavities Influence Dental Nerve Deterioration
Cavities are often underestimated in their ability to affect deeper structures. As bacteria gradually penetrate enamel and dentin, they release acids and metabolic byproducts. These substances diffuse toward the pulp and irritate the dental nerve long before the cavity becomes visible or painful. In many cases, low grade irritation continues for months or years, slowly weakening the nerve’s vitality.
Additionally, dentin contains tiny tubules that act like microscopic channels leading inward. As decay progresses, these tubules provide a pathway for external stimuli and bacterial toxins to move closer to the nerve. Individuals sometimes describe this stage as “occasional zingers” or sharp, brief sensations triggered by cold drinks. These early warnings show that the cavity’s progression is reaching the inner tissues. Without intervention, the pulp may eventually lose its ability to defend itself.
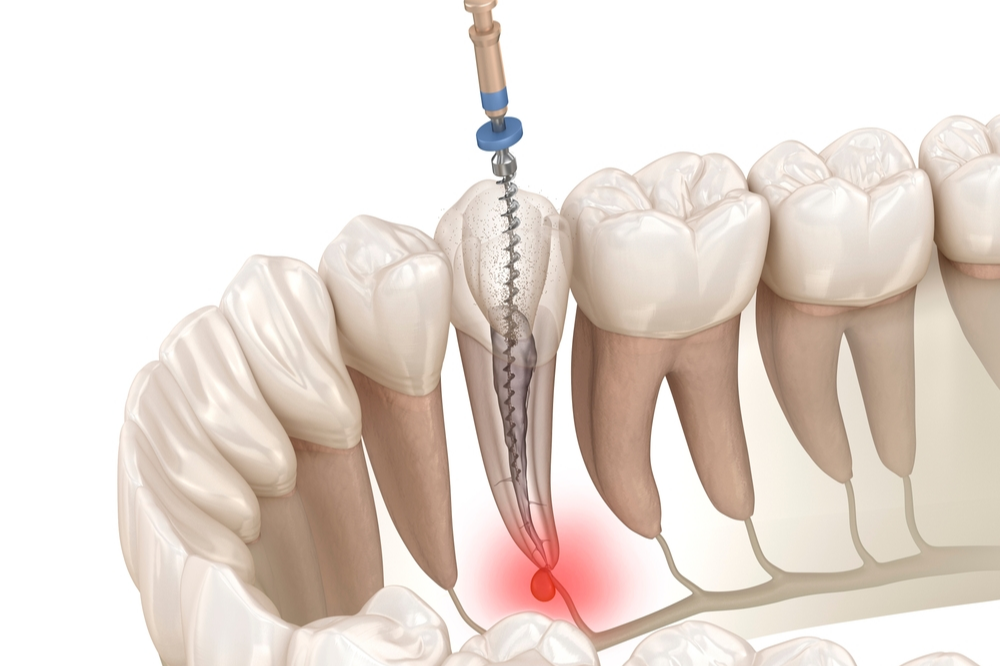
Temperature Sensitivity: A Window Into Dental Nerve Behavior
Temperature response is one of the most helpful clues when evaluating the condition of a tooth. The dental nerve contains specific fibers that react differently to cold and heat. When cold sensitivity increases unexpectedly, it may indicate inflammation inside the pulp chamber. In contrast, prolonged pain from heat often suggests reduced vitality.
Another fascinating factor is how temperature testing can reveal the stage of nerve decline. A tooth that reacts strongly to cold yet settles quickly may still have a functioning nerve. A tooth that shows delayed cooling response may be transitioning into a compromised state. These subtle patterns help professionals understand the timeline of nerve changes without invasive procedures.
Chemical Irritants and Their Silent Effects on the Dental Nerve
Everyday substances can influence nerve health more than people realize. Highly acidic drinks, aggressive whitening products, or deep restorations can irritate the inner dentin and gradually affect the pulp. Although these elements rarely cause immediate nerve death, they may contribute to chronic stress that accumulates over time. The dental nerve responds to pressure, chemical shifts, and pH variations, all of which add layers to the overall picture of nerve health.
Whitening agents, for example, can seep into dentin tubules and temporarily disturb the inner tissues. Many individuals feel short bursts of sensitivity after whitening sessions. While these sensations generally resolve, they highlight how reactive the nerve system is to external stimuli. Understanding this helps clarify why the pulp is vulnerable even during cosmetic procedures.
The Inflammatory Cycle Leading to Dental Nerve Breakdown
Inflammation is the central mechanism behind nerve damage. When the pulp becomes irritated, fluid accumulates inside an enclosed chamber with no ability to expand outward. Pressure builds, creating a hostile environment for the dental nerve. If this cycle continues without relief, the nerve begins losing vitality.
At the same time, inflammation changes the internal chemistry of the pulp, reducing oxygen levels and altering the nerve’s electrical behavior. People often describe this stage as having unpredictable pain sometimes intense, sometimes absent. This inconsistency reflects the nerve’s fluctuating ability to function under stress. Eventually, prolonged inflammation may push the pulp into a state where the nerve stops responding altogether.
How Restorative Procedures Occasionally Affect the Dental Nerve
Procedures such as fillings, crowns, or deep cleanings sometimes create temporary irritation in the inner tissues. Even with careful technique, vibration, heat, or slight pressure changes can influence the pulp chamber. The dental nerve may react with sensitivity that appears during biting or when exposed to temperature shifts.
Interestingly, post-treatment sensitivity often improves as the nerve adapts to the new environment. The pulp is capable of healing mild irritation and rebuilding its internal balance. But in rare cases, the irritation might exceed the body’s ability to recover, leading to longer term changes. Such outcomes provide insight into the nuanced relationship between dental procedures and nerve resilience.
The Unlikely Influence of Habitual Behaviors
Certain repetitive behaviors impact nerve function in subtle ways. Teeth grinding, clenching, or constant pressure on one side of the mouth can stress the internal structures over time. These habits create microtrauma that affects circulation and nerve responsiveness. The dental nerve may show heightened sensitivity during periods of increased tension, illustrating how behavioral patterns interact with biological systems.
People often overlook how nighttime habits, jaw posture, or even chewing style play roles in nerve health. These actions shape the mechanical environment surrounding the tooth, influencing how the pulp experiences pressure and vibration. Recognizing these factors allows for a more complete understanding of nerve behavior.
Understanding the Body’s Signals When Nerve Activity Declines
The moment the dental nerve begins to lose function, the body sends signals that often appear subtle at first. One of the most interesting aspects of nerve decline is how gradually these signs develop. Some individuals notice that a tooth no longer reacts to cold sensations the way it used to, or that pressure on the tooth feels strangely muted. These sensory changes reflect a shift in how the nerve transmits information. The tooth may still function during daily activities, yet internally the communication system is becoming increasingly quiet.
In some cases, discomfort becomes inconsistent. A tooth might feel completely normal one day and oddly heavy or dull the next. This inconsistency arises because the pulp tissue is undergoing a transformation that interferes with normal responsiveness. Even though these signals may not feel urgent, they often represent the later stages of nerve deterioration. The internal environment of the tooth continues to change until the nerve eventually becomes inactive.
How the Body Responds to a Silent Dental Nerve
Once the dental nerve stops reacting, the surrounding tissues begin adapting. The tooth no longer interprets temperature or pressure in a typical way, and individuals may find that the tooth blends into daily function without drawing attention. Although the absence of strong discomfort may feel reassuring, the biological activity inside the root system becomes more complex. Without nerve function, the inner chamber may undergo chemical changes that influence surrounding structures.
Interestingly, this stage sometimes creates a sense of “emptiness” or a muted sensation when chewing. While not a definitive indicator of nerve decline, this subtle change shows how closely sensory perception and nerve vitality are linked. The absence of active nerve signals shifts the way the tooth behaves within the broader system, demonstrating how interconnected the entire oral environment is.
What Happens Internally When Nerve Death Leads to Secondary Reactions
Once nerve activity ceases, other tissues inside the tooth begin adjusting to the new state. Although the tooth itself remains structurally intact, metabolic changes occur inside the pulp chamber. These internal shifts may cause the surrounding bone or ligament to compensate by altering the way they support the tooth. The dental nerve no longer regulates these systems, so the body relies on alternative pathways to maintain balance.
In some situations, the tooth becomes more vulnerable to changes in pressure from chewing or subtle temperature fluctuations. These shifts do not necessarily cause discomfort but reflect the absence of active nerve regulation. Because the tooth is still part of the broader biological network, any alteration in its internal environment influences the structures around it. Over time, these adjustments may become noticeable even without acute symptoms.
How Specialists Evaluate a Non Responsive Dental Nerve
When a tooth stops responding normally, specialists rely on a combination of sensory tests, structural assessments, and observational patterns to understand what is occurring. The dental nerve can behave unpredictably depending on the stage of deterioration, so evaluations focus on patterns rather than singular outcomes. Temperature tests, percussion responses, and visual changes all contribute to a clearer picture of nerve behavior.
These assessments do not provide absolute results but instead reveal how the tooth interacts with internal and external stimuli. For example, a delayed temperature response may suggest partial nerve activity, while a complete lack of sensation indicates that the pulp has entered a non vital state. Each clue contributes to a broader understanding of the tooth rather than providing a single definitive answer.
The Adaptive Phase: How a Tooth Behaves After Losing Nerve Function
A tooth without a functioning nerve does not immediately lose its role in daily chewing. Instead, the system adapts. The periodontal ligament still provides feedback, allowing the tooth to detect pressure at a basic level. The absence of the dental nerve means the tooth can no longer sense subtle temperature variations, but structural function remains relatively stable. Individuals often continue using the tooth without major disruptions.
However, the inner tissues, now inactive, may begin to shift chemically. The pulp chamber changes consistency over time, and the tooth becomes more reliant on external structures for support. Some individuals describe a vague sense of difference when biting or a slight change in the sound produced when tapping the tooth. These observations reveal how interconnected sensory systems continue functioning even after nerve activity fades.
Long Term Considerations After Dental Nerve Decline
When the nerve becomes inactive, the biological dynamics around the tooth evolve over months or years. The internal chamber no longer receives the same metabolic support it once did, leading to changes in the internal composition. While the tooth remains part of the functional chewing system, the absence of nerve regulation may impact how it interacts with routine stimuli.
People occasionally notice that the tooth takes on a slightly different tone or shading over extended periods. This shift often reflects internal changes rather than external damage. Although these visual cues are subtle, they provide insight into how the inner structures transform once nerve activity diminishes. The dental nerve no longer influences internal circulation, and the tooth gradually adapts to a more static state.
When a Non Vital Tooth Requires Future Intervention
Although a tooth without nerve activity may remain functional for a long time, certain changes can signal the need for future evaluation. These changes tend to appear as the internal environment shifts and the surrounding tissues respond. Specialists observe structural resilience, sensitivity patterns, and external changes to determine whether intervention may be helpful.
It is the gradual nature of these shifts that makes them so significant. The tooth often continues performing its role while internal changes accumulate quietly. Understanding these stages highlights how the absence of a dental nerve influences the tooth in the long term. It also provides a clearer picture of how the body adapts and how stability is maintained even when the natural sensory system is no longer active.