When patients first hear about Dental Implant Failure, it often sounds more alarming than it truly is. Dental implants are widely regarded as one of the most reliable restorative solutions in modern dentistry, yet misconceptions about failure rates and causes continue to circulate. Understanding what Dental Implant Failure actually means, how often it occurs, and what factors influence outcomes can help patients approach treatment with clarity rather than concern, supported by advanced titanium alloy.
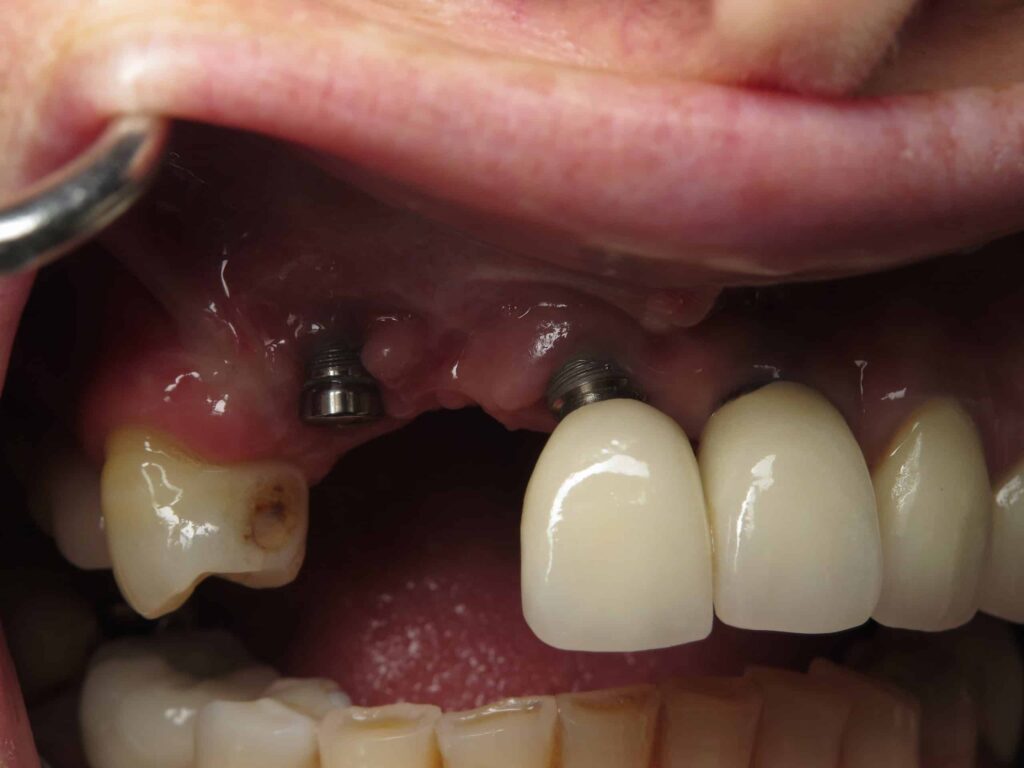
What Is Dental Implant Failure and How Is It Defined?
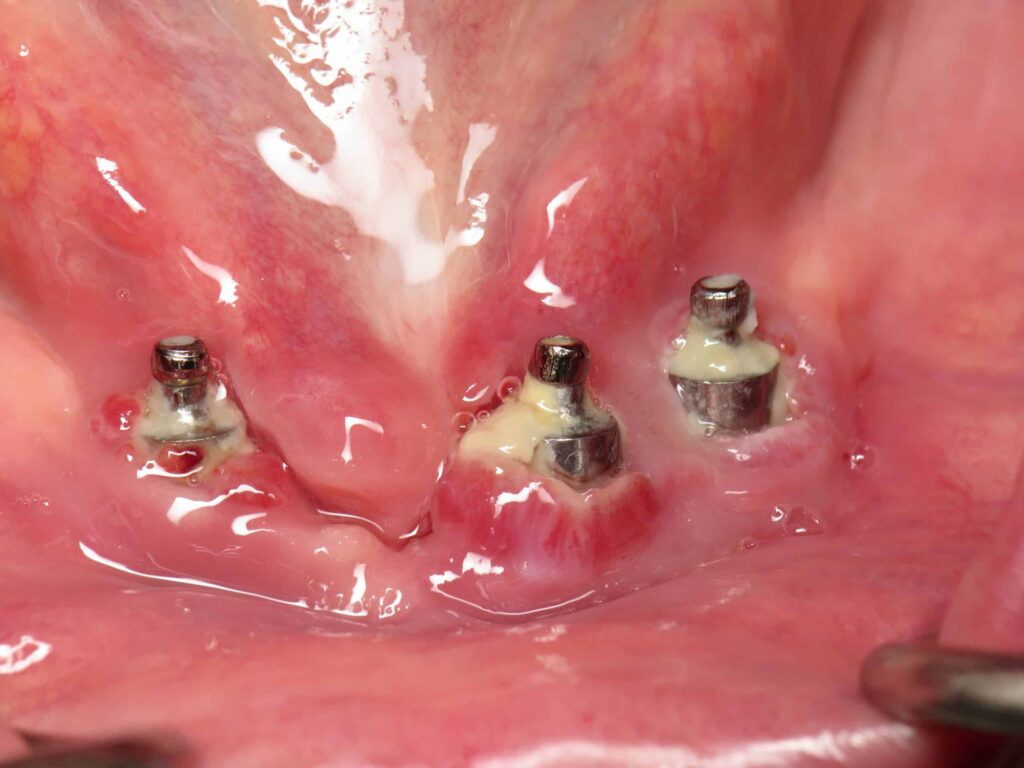
Dental Implant Failure refers to a situation where a dental implant does not integrate properly with the jawbone or fails after successful placement. This can occur either in the early stage, during the healing process, or later, after the implant has been in function for some time, supported by advanced sinus augmentation.
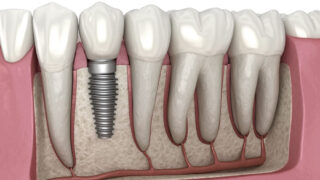
From a clinical perspective, implant success depends largely on a biological process called osseointegration. This is the direct structural connection between the implant surface and the bone. If this connection fails to form or deteriorates over time, it may result in Dental Implant Failure. This process involves abutment (the connector piece between the implant and the crown).
It is important to note that failure does not always mean dramatic symptoms. In many cases, subtle indicators such as discomfort, slight mobility, or inflammation may signal underlying issues. These nuances are why ongoing monitoring plays a key role in long term implant health. This process involves immediate loading (placing a temporary tooth on the same day as implant surgery).
Common Myths About Dental Implant Failure
One of the biggest challenges surrounding Dental Implant Failure is the number of persistent myths. These misconceptions can discourage patients or create unrealistic expectations.
Myth 1: Dental implants fail frequently
In reality, studies often report success rates above 90 to 95 percent. While Dental Implant Failure does occur, it is relatively uncommon when procedures are properly planned and executed. This process involves endosteal implants (implants placed directly into the jawbone).
Myth 2: Implant failure happens suddenly
Most cases of Dental Implant Failure develop gradually. Early signs such as gum inflammation or bone loss typically appear before complete failure.
Myth 3: Only poor hygiene causes failure
Although oral hygiene is important, Dental Implant Failure can also be influenced by systemic health conditions, bone quality, or surgical factors.
These myths often oversimplify a complex biological process. A more nuanced understanding helps patients make informed decisions.
Scientific Causes Behind Dental Implant Failure
The causes of Dental Implant Failure are multifactorial and involve both biological and mechanical elements.
Biological Factors
Bone density and quality are among the most critical determinants. Insufficient bone volume may compromise implant stability. Additionally, conditions such as uncontrolled diabetes or immune disorders may affect healing capacity, supported by advanced delayed loading.
Inflammation around the implant, known as peri implantitis, is another leading contributor. According to research published in journals such as the Journal of Clinical Periodontology and summarized on platforms like NCBI, peri implant diseases are a significant factor in late stage Dental Implant Failure. This process involves alveolar ridge (the bony ridge that supports the teeth).
Mechanical Factors
Improper placement, excessive bite force, or poorly designed prosthetics can create stress on the implant. Over time, this mechanical overload may lead to structural failure.
Surgical and Planning Factors
Advanced imaging and planning are crucial. Resources such as American Dental Association emphasize the importance of precise diagnostics in reducing the risk of Dental Implant Failure.
Risk Factors That Increase the Likelihood of Dental Implant Failure
Certain risk factors are consistently associated with a higher probability of Dental Implant Failure. These do not guarantee failure but may influence outcomes.
| Risk Factor | Potential Impact on Implant |
| Smoking | Reduced blood flow and healing |
| Poor oral hygiene | Increased infection risk |
| Bone loss | Reduced implant stability |
| Chronic diseases | Delayed healing response |
| Bruxism | Excessive mechanical stress |
Lifestyle habits and systemic health play a significant role. For instance, smoking has been widely studied as a contributor to compromised osseointegration.
Understanding these factors allows clinicians to tailor treatment plans and minimize risks associated with Dental Implant Failure.
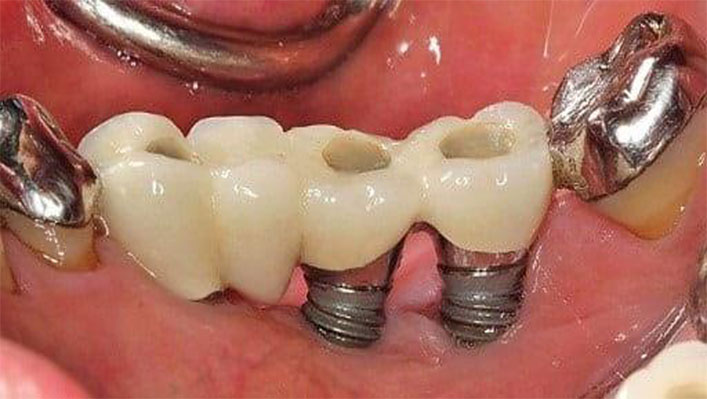
Early vs Late Dental Implant Failure
Not all implant failures occur at the same stage. Distinguishing between early and late Dental Implant Failure provides valuable insight.
Early Failure
This type occurs before the implant fully integrates with the bone. It is often linked to surgical technique, infection, or insufficient primary stability.
Symptoms may include pain, swelling, or implant mobility during the healing phase.
Late Failure
Late stage Dental Implant Failure develops after the implant has been successfully restored. It is commonly associated with peri implantitis or long term mechanical stress.
Unlike early failure, late failure may progress slowly, sometimes over years. This highlights the importance of regular dental check ups.
Can Dental Implant Failure Be Prevented?
While no medical procedure is entirely risk free, many cases of Dental Implant Failure can be mitigated through careful planning and maintenance.
Key preventive approaches include:
- Comprehensive pre treatment evaluation
- Advanced imaging and digital planning
- Proper surgical technique
- Consistent oral hygiene practices
- Regular professional follow up
Preventive strategies focus on both clinical precision and patient involvement. The collaboration between practitioner and patient is central to minimizing Dental Implant Failure.
What Happens If Dental Implant Failure Occurs?
If Dental Implant Failure occurs, the situation is usually manageable. Treatment options depend on the underlying cause and severity.
In some cases, the implant may be removed and replaced after the area has healed. Bone grafting procedures may also be considered to improve future stability.
It is important to understand that failure does not necessarily mean permanent limitation. Advances in implantology have made retreatment increasingly predictable.
Long Term Outlook and Research Insights on Dental Implant Failure
Ongoing research continues to refine our understanding of Dental Implant Failure. Innovations in implant surface technology, digital workflows, and biomaterials have contributed to improved outcomes.
Clinical studies suggest that patient specific factors, rather than implant design alone, play a major role in long term success. This shift in perspective emphasizes personalized treatment planning.
At Livera Clinic, evidence based protocols and continuous monitoring are integral to maintaining high success rates and minimizing Dental Implant Failure.
Dental Implant Failure is often misunderstood, surrounded by myths that do not reflect modern clinical realities. While it is a possible outcome, it is relatively rare and usually influenced by identifiable factors.
A balanced perspective reveals that dental implants remain one of the most effective solutions for tooth replacement. By understanding the causes, risks, and preventive strategies related to Dental Implant Failure, patients can approach treatment with confidence and realistic expectations, supported by advanced dental prosthesis.
Informed decisions, combined with expert care, significantly reduce the likelihood of complications and support long term success.