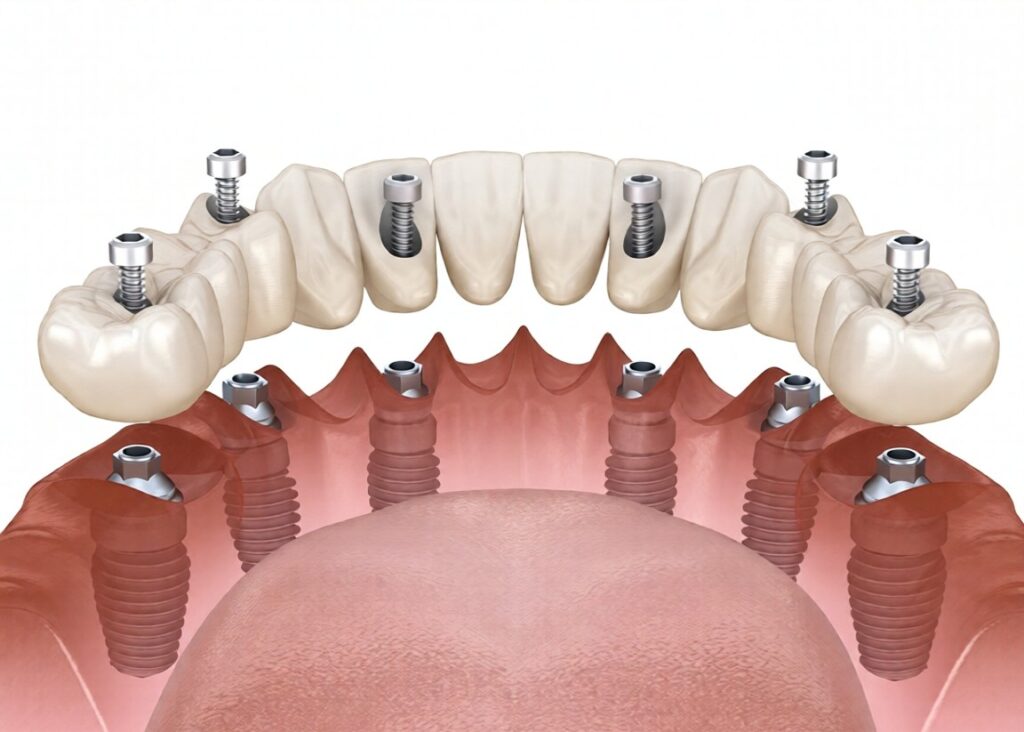
Losing a tooth can feel like a tiny architectural crisis inside the mouth. Chewing changes, speech may shift, and confidence often takes an unnecessary hit. That is one reason Dental Implants have become one of the most discussed restorative options in modern dentistry. Yet while many people focus on the final result the natural-looking crown and renewed bite the real story unfolds underneath the surface, where bone, gum tissue, and biology work together through a carefully timed healing process, supported by advanced dental prosthesis.
At Livera Clinic, we know that people are rarely curious about the titanium post alone. What they really want to understand is what happens after placement, how long healing may take, why one stage feels uneventful while another seems slow, and what “successful integration” actually means. The healing journey of Dental Implants is not a single event but a sequence of biological stages. Each one contributes to stability, comfort, and long-term function. Understanding these stages can make the whole process feel less mysterious and far more logical. This process involves alveolar ridge (the bony ridge that supports the teeth).
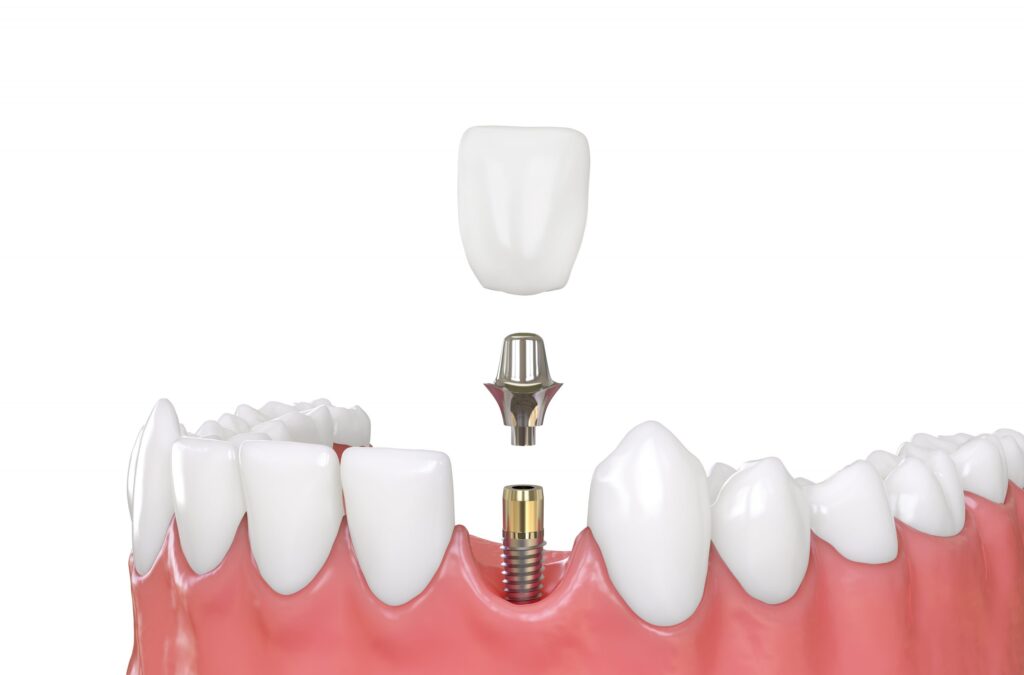
Understanding How Dental Implants Heal in the Body
Healing around Dental Implants is often described as a blend of surgery recovery and tissue engineering. Unlike a filling or crown that sits on existing tooth structure, an implant becomes part of the jaw environment. That means the body does not simply “close the wound.” It must also adapt to a new material and build a stable relationship between implant surface, surrounding bone, and soft tissue.
This process is commonly called osseointegration. The term sounds highly technical, but the basic idea is straightforward: the bone gradually heals around the implant and forms a firm structural bond. Researchers have long examined how implant surface texture, bone quality, surgical technique, and general health patterns may affect this phase. While healing timelines vary, the biological pattern tends to follow recognizable stages. That is why Dental Implants are often discussed not as a one-day treatment, but as a treatment with a healing roadmap, supported by advanced titanium alloy.
The First Stage of Dental Implants Healing: Immediate Post-Surgical Response
The earliest stage begins right after implant placement. At this point, the body reacts much like it would after any controlled surgical procedure. Blood clot formation occurs around the implant site, and this is not a problem to be avoided it is actually a useful biological starting point. The clot helps protect the site and creates the conditions for early tissue repair.
Inflammation follows, but in a normal healing context, inflammation is not automatically negative. It is part of the body’s communication system. Cells involved in cleanup and repair begin working in the area, removing damaged tissue and preparing for regeneration. In the first few days, people may notice mild swelling, tenderness, or changes in chewing comfort. These short-term responses do not define the final outcome of Dental Implants. They are simply the opening chapter of healing, supported by advanced sinus augmentation.
At the same time, the implant is mechanically stable because it has been placed into bone, but biological stability is still developing. That distinction matters. Early on, the implant may feel “in place,” yet the deeper bond with bone is still forming. This is why the first stage is less about visible change and more about microscopic activity.
Soft Tissue Recovery Around Dental Implants
Once the initial surgical response settles, the gums begin a more organized phase of repair. Soft tissue healing around Dental Implants plays a major role in both aesthetics and protection. Healthy gum adaptation can help create a seal around the implant area, which may reduce the likelihood of irritation from bacteria and food debris.
This phase is often underestimated because people tend to focus on bone. However, the soft tissue frame around implant-supported restorations matters enormously. The gum contour influences how natural the final result appears, especially in visible areas such as the front teeth. It also affects long-term hygiene access. If the tissues heal neatly and adapt well, the implant site is often easier to maintain.
The timing of soft tissue healing can differ depending on whether the implant was placed immediately after extraction, whether a graft was involved, and whether a temporary restoration is used. In many cases, gum tissue appears to improve faster than bone, but appearances can be deceptive. A site may look calm while deeper healing is still in progress. That is one reason clinicians evaluate Dental Implants in stages rather than by surface appearance alone. This process involves immediate loading (placing a temporary tooth on the same day as implant surgery).
Bone Healing and Osseointegration in Dental Implants
This is the phase most people mean when they ask whether an implant has “healed.” Bone healing around Dental Implants is the core biological event that supports long-term function. During osseointegration, the surrounding bone remodels and adapts to the implant surface. Early woven bone may form first, then gradually mature into stronger lamellar bone over time.
From a scientific perspective, this stage is dynamic rather than linear. Bone cells do not merely fill a gap; they respond to mechanical conditions, blood supply, implant design, and the condition of the host bone. Studies over the years have suggested that implant surface technologies may support faster or more predictable early integration in some cases, although outcomes still depend on multiple factors rather than one feature alone, supported by advanced delayed loading.
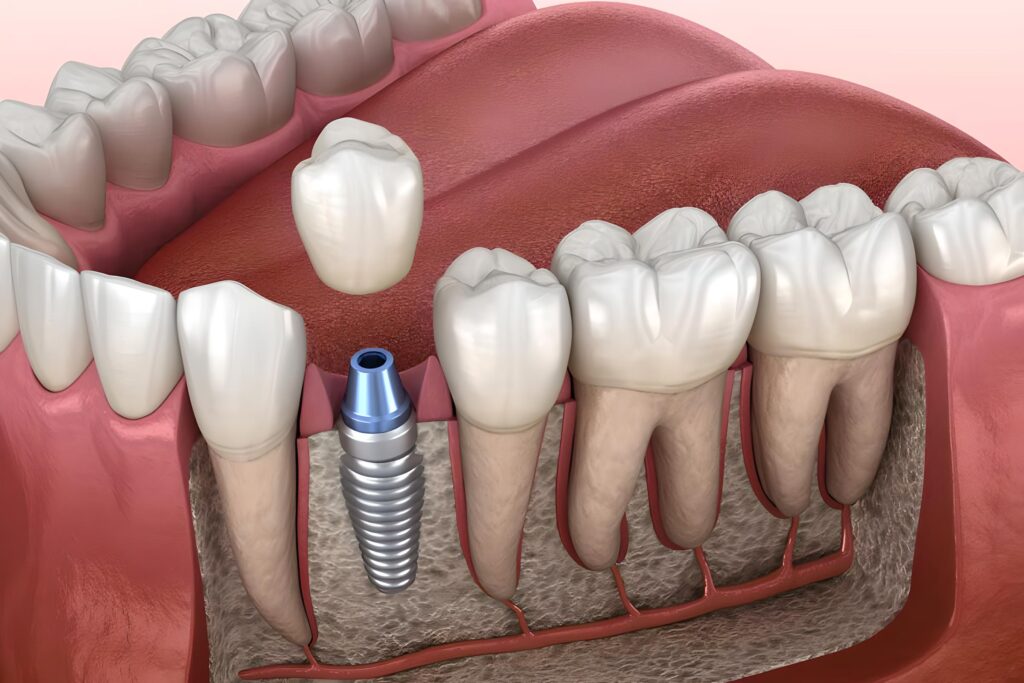
A useful way to think about this stage is to imagine scaffolding around a building. In the beginning, the structure is being supported while permanent reinforcements are installed. Over time, the support system is replaced by a stronger, more stable framework. That is roughly how Dental Implants become functionally anchored. The transformation is mostly invisible, but biologically it is the centerpiece of the entire treatment. This process involves endosteal implants (implants placed directly into the jawbone).
Below is a simple overview of the healing stages:
| Healing Stage | What Happens Biologically | What It May Mean Clinically |
| Immediate response | Blood clot forms, inflammation begins | Early tenderness, swelling, site protection |
| Soft tissue repair | Gum tissue closes and adapts | Improved comfort, better tissue contour |
| Osseointegration | Bone attaches and remodels around implant | Increasing stability over time |
| Functional adaptation | Implant begins handling bite forces | Transition toward long-term use |
| Long-term maintenance | Bone and gum balance are preserved | Ongoing monitoring and hygiene matter |
What Can Influence the Healing Time of Dental Implants?
Healing is biological, but it is not identical for everyone. The timeline for Dental Implants may be shaped by several overlapping factors. Bone density is one of the most discussed. Dense bone may provide strong initial fixation, while softer bone may require a more cautious healing strategy. This does not mean one situation is “good” and the other is “bad.” It simply means the healing plan may differ.
General oral conditions can also play a role. The health of the gums, the presence of previous infection, and whether bone grafting was needed may all influence the pace of recovery. Lifestyle patterns are frequently mentioned in implant literature as well. Habits that affect circulation, tissue recovery, or oral hygiene routines may shape the healing environment around implant-supported restorations.
Other variables include:
- Implant location in the upper or lower jaw
- Whether extraction and implant placement happened at the same time
- The need for sinus lift or grafting procedures
- Bite pressure and parafunctional habits such as grinding
- The timing of temporary or permanent restoration placement
Because of these differences, comparisons between patients can be misleading. One person’s Dental Implants may be restored relatively quickly, while another may need a longer observation period. That is not necessarily a sign of complication. Often, it simply reflects personalized treatment planning.
The Transition Stage: When Dental Implants Begin Functional Loading
At some point, healing moves from a sheltered biological phase into a mechanical one. This is when Dental Implants begin to participate in function, either through a temporary or final prosthetic restoration. Functional loading means the implant is no longer just healing quietly in bone; it is starting to experience chewing forces and daily use.
This stage is important because the implant-bone relationship must now perform, not just exist. In well-planned cases, controlled loading may help confirm that integration is progressing in a favorable way. Yet the timing of this step can vary widely. Some implants are restored earlier under specific conditions, while others are left unloaded longer to support more conservative healing.
The concept often sounds dramatic, but it is really about adaptation. Just as muscles respond to exercise and bones respond to pressure, implant-supported structures respond to function. The key is balance. Excessive force too early may be less ideal than gradual, well-managed loading. That is why the transition phase of Dental Implants is usually guided by clinical assessment rather than a fixed universal calendar.
Signs That Healing of Dental Implants Is Progressing Normally
People often expect healing to announce itself with a dramatic “all clear” moment. In reality, progress with Dental Implants is often quiet. Normal healing may look like reduced tenderness, stable gum appearance, absence of persistent swelling, and increasing comfort with routine mouth function. The site may gradually feel less like a treated area and more like a natural part of the mouth.
However, normal healing is not always identical to symptom-free healing. Minor sensitivity, slight tissue awareness, or temporary chewing caution may occur during recovery. What matters more is the overall pattern. Is the area becoming more stable over time? Is the tissue settling rather than worsening? Is the implant being monitored appropriately? These are the kinds of questions clinicians typically consider.
From a scientific viewpoint, radiographic evaluation and clinical stability checks often provide more useful insight than sensation alone. Bone changes are not usually something a person can feel directly. That is another reason the healing of Dental Implants should be understood as both a personal experience and a clinical process.
Long-Term Tissue Adaptation After Dental Implants Healing
Healing does not truly end the day the final crown is placed. After Dental Implants have integrated and become functional, the surrounding bone and soft tissue continue to adapt. This later phase is less about recovery from surgery and more about achieving equilibrium. The mouth is a living system, not a static display case, so tissues respond over time to cleaning habits, bite force, gum health, and restoration design, supported by advanced zygomatic implants.
Long-term success is often linked to how well the implant environment remains balanced. The gum margin should be maintainable. The restoration should be shaped in a way that allows cleaning. The bite should distribute force reasonably. Scientific discussions on implant longevity frequently focus on these maintenance-related variables because biology does not stop once the implant is restored.
For that reason, the story of Dental Implants is best told in two parts: healing and stewardship. The first builds the foundation. The second protects it. When people understand this, they are less likely to see implant treatment as a single procedure and more likely to recognize it as a carefully staged oral rehabilitation process.
Why the Healing Journey of Dental Implants Deserves Patience
The healing stages of Dental Implants reveal something fascinating about modern dentistry: success depends as much on biology as on technology. Titanium, surface engineering, digital planning, and restorative design all matter. But ultimately, the body must do the quiet, intricate work of repair, integration, and adaptation. That work happens in phases, and each phase has its own purpose.
For many people, understanding those stages makes the process feel less intimidating. The first stage is protection. The second is tissue repair. The third is osseointegration. The fourth is functional adaptation. The fifth is long-term stability. Seen this way, implant healing is not mysterious at all. It is simply structured, gradual, and deeply biological.
At Livera Clinic, we believe informed patients make calmer, more confident decisions. That is why learning how Dental Implants heal can be just as valuable as learning how they look. When the journey is understood, the waiting becomes more meaningful, and the result feels less like a quick fix and more like a carefully built restoration.