Gum Graft procedures are among the most studied and refined periodontal techniques for managing gum recession and improving soft tissue stability around teeth. At Livera Clinic, the concept of a Gum Graft is approached not as a cosmetic shortcut, but as a biologically driven periodontal intervention designed to support long term oral health, tissue harmony, and functional balance.
Gum recession may develop gradually due to periodontal inflammation, mechanical trauma, genetic predisposition, orthodontic movement, or thin gingival biotype. When roots become exposed, patients often report sensitivity, aesthetic concerns, and difficulty maintaining hygiene. A carefully planned Gum Graft can help reinforce the gingival margin, improve root coverage, and enhance soft tissue thickness.

What Is a Gum Graft and Why Is It Performed?
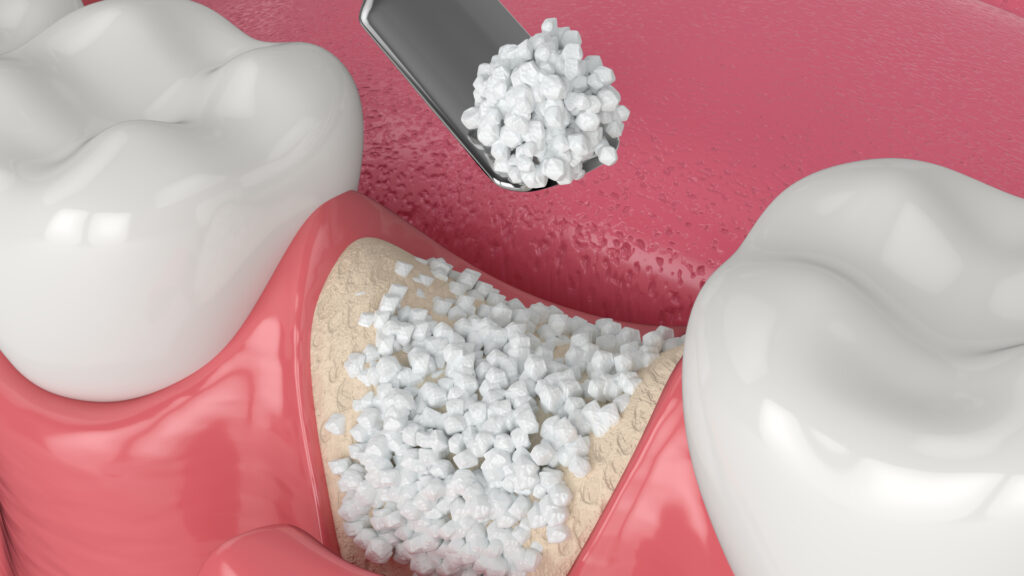
A Gum Graft is a periodontal surgical procedure designed to add or reposition gum tissue in areas where recession has exposed the tooth root. The main objective is to increase the width or thickness of keratinized tissue and potentially reduce root hypersensitivity. In clinical terminology, this may also be described as gingival grafting, soft tissue grafting, or periodontal plastic surgery.
Periodontal research suggests that tissue stability is influenced by multiple variables, including biotype thickness, plaque control, occlusal forces, and inflammatory history. While not every case of recession requires intervention, a Gum Graft may be considered when progressive tissue loss, aesthetic imbalance, or structural vulnerability is observed. The decision is typically based on clinical evaluation rather than cosmetic preference alone.
Biological Principles Behind Gum Graft Healing
Understanding the biology of a Gum Graft provides insight into why technique selection matters. Grafted tissue survives through plasmatic diffusion during the initial phase, followed by revascularization and integration with the recipient site. Blood supply, tissue thickness, and surgical precision significantly influence outcomes.
Soft tissue grafting is supported by decades of periodontal literature examining epithelial and connective tissue behavior. Connective tissue grafts, for instance, are often associated with predictable root coverage because of their dual blood supply. However, healing responses vary between individuals. Factors such as smoking status, systemic health, and oral hygiene practices can influence post operative tissue adaptation.
Types of Gum Graft Techniques Used in Modern Dentistry
Different Gum Graft techniques are selected based on clinical goals and anatomical conditions. Below is a structured comparison of commonly used approaches:
| Technique | Tissue Source | Main Objective | Typical Indications |
| Connective Tissue Graft | Palatal connective tissue | Root coverage and thickness increase | Localized recession |
| Free Gingival Graft | Surface palatal tissue | Increase keratinized tissue width | Minimal attached gingiva |
| Pedicle Graft | Adjacent gum tissue | Root coverage with preserved blood supply | Isolated defects |
| Allograft or Xenograft | Donor biomaterial | Avoid secondary donor site | Patients preferring minimally invasive approach |
Each Gum Graft method has advantages and limitations. For example, connective tissue grafts are widely documented for aesthetic blending, while free gingival grafts may prioritize functional tissue gain. Biomaterial alternatives may reduce surgical morbidity but depend on case specific biological response.
Step by Step Overview of a Gum Graft Procedure
A Gum Graft procedure generally begins with a detailed periodontal assessment. Measurements of recession depth, tissue thickness, keratinized gingiva width, and bone levels are evaluated. Photographic documentation and digital scans may assist in treatment planning.
During surgery, the recipient site is carefully prepared to create a vascular bed. The graft tissue, whether autogenous or biomaterial based, is positioned and stabilized with micro sutures. The precision of adaptation plays a critical role in healing. After placement, protective measures may be used to support clot stability.
Post operative healing evolves in phases:
- Initial clot stabilization
- Early revascularization
- Epithelial maturation
- Long term tissue remodeling
While patients often notice visual improvement within weeks, full biological integration may take several months. Each Gum Graft should be viewed as a gradual regenerative process rather than an instant transformation.

Clinical Outcomes and Long Term Stability of Gum Graft Procedures
Scientific literature often evaluates Gum Graft success based on root coverage percentage, keratinized tissue gain, and patient satisfaction. Long term follow up studies suggest that stability depends heavily on plaque control and maintenance care.
It is important to recognize that no periodontal procedure guarantees identical outcomes for every patient. Variations in anatomy, immune response, and behavioral factors influence results. In well selected cases, a Gum Graft may contribute to improved tissue resilience and aesthetic harmony. However, long term success relies on consistent monitoring and preventive strategies.
At Livera Clinic, documentation protocols and follow up assessments are integrated into treatment philosophy. This approach aims to align biological understanding with patient centered expectations.
Comparing Gum Graft With Alternative Recession Treatments
Not all recession defects require a Gum Graft. In certain scenarios, desensitizing agents, composite bonding, or orthodontic adjustments may be explored. The choice depends on defect classification, bone support, and aesthetic priorities.
For example, mild recession without inflammation may remain stable for years under proper hygiene supervision. In contrast, progressive recession with thin biotype might benefit from soft tissue reinforcement. A Gum Graft is typically considered when structural reinforcement is preferred over symptomatic management alone.
From a scientific perspective, treatment planning often references Miller or Cairo recession classifications. These systems help estimate potential root coverage outcomes and guide procedural selection.
Risk Factors and Considerations in Gum Graft Planning
Every Gum Graft requires careful case evaluation. Potential influencing factors include:
- Gingival biotype thickness
- Smoking habits
- Bruxism and occlusal stress
- Systemic inflammatory conditions
- Plaque accumulation patterns
Research indicates that smoking may reduce vascular response, potentially affecting graft integration. Similarly, uncontrolled inflammation may compromise tissue adaptation. Therefore, preparatory periodontal therapy is often emphasized before performing a Gum Graft.
Patient communication is also essential. Expectations should align with anatomical reality. While aesthetic improvement is often achieved, the primary objective remains structural reinforcement and periodontal stability.
The Role of Technology in Modern Gum Graft Techniques
Advancements in microsurgical instruments, magnification systems, and biomaterials have influenced how a Gum Graft is performed today. Microsurgical approaches aim to reduce tissue trauma and enhance precision in suturing.
Digital imaging and intraoral scanning allow clinicians to evaluate recession patterns with greater accuracy. These technologies do not replace surgical expertise but may enhance diagnostic clarity. A Gum Graft supported by careful planning and magnification may offer improved tissue adaptation compared to traditional macroscopic techniques.
Biomaterial research continues to evolve, with collagen matrices and growth factor enhanced membranes being explored. While promising, long term comparative studies are still developing.
Scientific Perspective on Gum Graft Procedures
A well indicated Gum Graft can serve as a biologically grounded solution for gum recession management. Rather than viewing it solely as a cosmetic enhancement, it is more accurately described as a periodontal reinforcement strategy. By increasing tissue thickness and potentially covering exposed roots, grafting procedures may contribute to improved structural balance.
At Livera Clinic, periodontal interventions are guided by evidence informed protocols, individualized planning, and long term maintenance philosophy. Each Gum Graft is evaluated within the broader context of oral health, anatomical factors, and patient expectations.
Soft tissue grafting continues to evolve through research, clinical innovation, and interdisciplinary collaboration. While outcomes vary, the principles of vascular supply, tissue adaptation, and inflammation control remain central. For individuals exploring periodontal solutions, understanding the science behind a Gum Graft can provide clarity and realistic perspective.