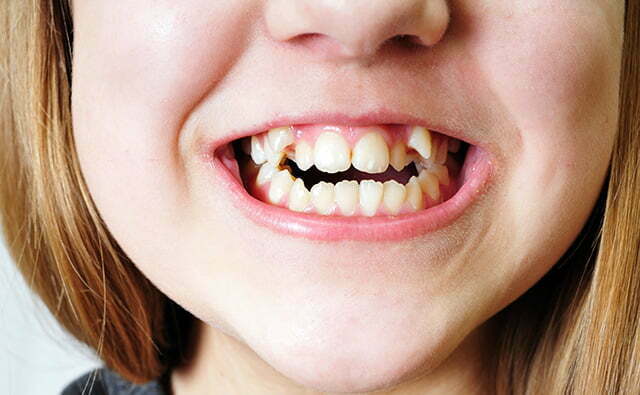
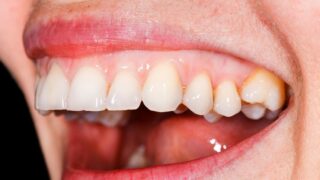
Malocclusion is a clinical term describing misalignment between the upper and lower dental arches, yet its meaning extends far beyond crooked teeth. In dental science, Malocclusion reflects the relationship between skeletal growth, tooth positioning, muscular balance, and functional bite harmony. While many people associate it primarily with orthodontic treatment, the topic encompasses structural biology, craniofacial development, and long term oral health dynamics.
This comprehensive guide explores the types, underlying causes, financial considerations, and broader implications of Malocclusion. Rather than reducing the topic to cosmetic correction, it examines the condition through a scientific and analytical lens, presenting insights grounded in orthodontic research and developmental biology.
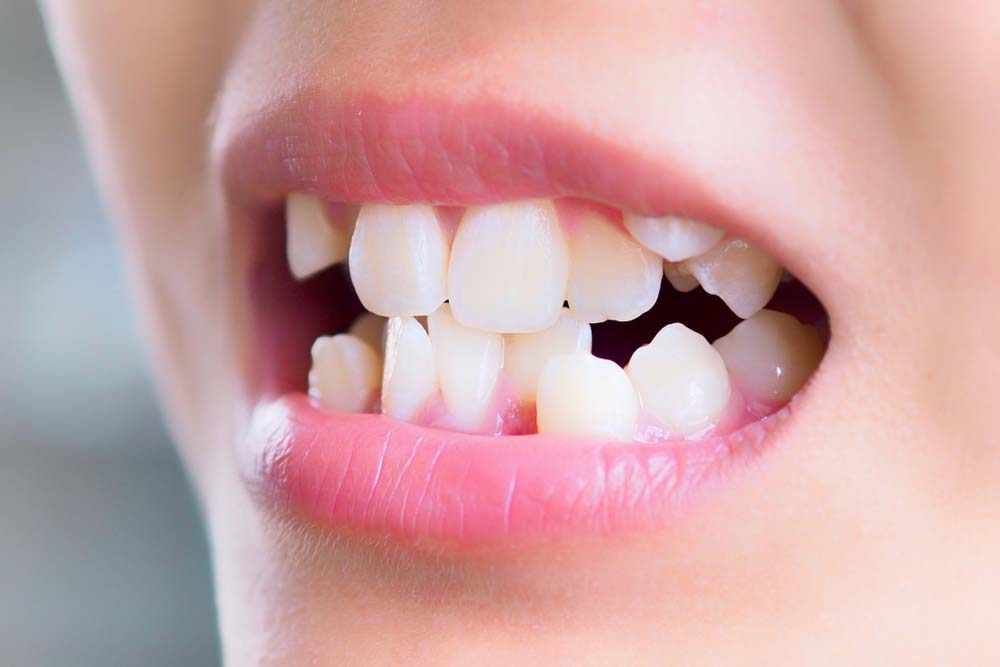
Understanding Malocclusion in Dental Science
In its simplest definition, Malocclusion describes an improper alignment of teeth when the jaws close. In ideal occlusion, upper teeth overlap lower teeth slightly, distributing chewing forces evenly across the dental arches. When this balance is disrupted, bite irregularities may emerge. However, the biological story of Malocclusion is more intricate than alignment alone.
Craniofacial growth plays a central role in the development of Malocclusion. During childhood and adolescence, jawbones grow in response to genetic instructions and environmental influences. Teeth erupt into spaces shaped by these skeletal frameworks. If jaw growth is disproportionate or tooth size exceeds available space, dental misalignment can result. Research in orthodontics consistently suggests that Malocclusion often reflects a mismatch between tooth dimensions and jaw capacity rather than a single isolated factor.
Types of Malocclusion and Bite Patterns
Dental professionals classify Malocclusion into several categories based on how the upper and lower molars relate to one another. Class I patterns generally involve normal molar relationships accompanied by crowding or spacing irregularities. Although considered the mildest form of Malocclusion, it can still influence aesthetics and oral hygiene efficiency.
Class II patterns are frequently associated with an overbite, where the upper jaw projects forward relative to the lower jaw. This type of Malocclusion may reflect skeletal discrepancies or dental protrusion. In contrast, Class III patterns involve a more prominent lower jaw, commonly described as an underbite. Skeletal Class III Malocclusion can influence facial profile and jaw symmetry.
Beyond these classifications, variations such as open bite, crossbite, and deep bite illustrate the complexity of dental misalignment. Each presentation of Malocclusion carries distinct structural characteristics, demonstrating that occlusal patterns exist along a spectrum rather than within rigid boundaries.
Causes of Malocclusion: Genetics and Growth Dynamics
The origins of Malocclusion are widely recognized as multifactorial. Genetic inheritance plays a significant role, particularly in jaw size, facial proportions, and tooth dimensions. Studies in craniofacial genetics indicate that individuals may inherit a tendency toward skeletal imbalance, increasing the likelihood of developing Malocclusion.
Environmental factors, however, are equally relevant. Early childhood behaviors such as prolonged thumb sucking or pacifier use may influence jaw growth direction. Chronic mouth breathing, often associated with airway issues, has been explored in research as a potential contributor to altered facial development patterns linked to Malocclusion. Additionally, premature loss of primary teeth can disrupt eruption pathways, creating space discrepancies that affect permanent alignment.
Anthropological findings also offer intriguing insights. Some researchers suggest that softer modern diets may reduce mechanical stimulation of the jaws during growth. Reduced functional demand could theoretically influence arch development and increase susceptibility to Malocclusion in contemporary populations.
Functional and Aesthetic Dimensions of Malocclusion
Although Malocclusion is frequently discussed in cosmetic terms, its functional aspects deserve equal attention. Bite imbalance can influence chewing efficiency and speech articulation. Uneven contact points may alter force distribution across the teeth, potentially affecting long term dental wear patterns.
From a biomechanical perspective, researchers have explored how Malocclusion interacts with temporomandibular joint dynamics. While not every case results in discomfort, irregular bite patterns may contribute to functional strain in certain individuals. Scientific literature continues to evaluate these correlations without drawing universal conclusions.
Facial symmetry is another dimension connected to Malocclusion. Dental alignment contributes to lower facial proportions and overall profile balance. Because teeth support soft tissue structures, changes in occlusion can subtly influence facial aesthetics. This dual functional and visual impact explains why Malocclusion remains a central topic in orthodontic research.
Diagnostic Evaluation of Malocclusion
The assessment of Malocclusion typically begins with a detailed clinical examination. Dental professionals evaluate bite relationships, tooth spacing, jaw symmetry, and facial proportions. Radiographic imaging such as panoramic and cephalometric scans allows precise measurement of skeletal angles and growth patterns.
Modern diagnostic tools have enhanced the understanding of Malocclusion. Three dimensional imaging and digital modeling technologies enable more accurate visualization of occlusal relationships. These tools assist clinicians in distinguishing between dental and skeletal forms of Malocclusion, which may influence management approaches.
Despite technological advances, interpretation remains individualized. Each case reflects a unique anatomical structure shaped by genetics and development. Therefore, the evaluation of Malocclusion requires comprehensive analysis rather than reliance on standardized templates.
Treatment Approaches for Malocclusion
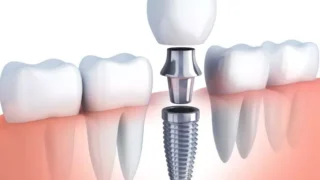
Management strategies for Malocclusion vary according to severity and structural origin. Orthodontic appliances such as fixed braces or clear aligners aim to gradually reposition teeth within the dental arches. These approaches primarily address dental forms of Malocclusion.
In growing adolescents, functional appliances may influence jaw development. By guiding skeletal growth, these devices attempt to modify underlying discrepancies associated with Malocclusion. In more complex skeletal cases, orthognathic surgery combined with orthodontic therapy may be considered. Such interventions reflect the intersection between dental alignment and craniofacial surgery.
The duration and complexity of Malocclusion treatment depend on biological response and growth stage. Research indicates that tooth movement relies on bone remodeling processes, which vary among individuals. Consequently, timelines cannot be generalized across all cases.
Expenses and Costs of Addressing Malocclusion
Financial considerations often arise when discussing Malocclusion. Treatment expenses differ based on geographic location, technological resources, and complexity of alignment. Mild dental Malocclusion may involve shorter treatment durations, whereas skeletal discrepancies requiring multidisciplinary care can increase overall costs.
Orthodontic technology also influences financial structure. Advanced imaging systems, customized aligner fabrication, and digital planning tools contribute to comprehensive diagnostic precision. These elements may affect the total cost associated with correcting Malocclusion.
Insurance policies vary internationally. In some healthcare systems, functional impairment linked to Malocclusion may influence reimbursement criteria. In others, orthodontic treatment is categorized primarily as elective. Therefore, understanding cost considerations involves evaluating clinical complexity alongside regional healthcare frameworks.
Long Term Outlook and Stability
The conclusion of active treatment does not necessarily mark the end of the Malocclusion journey. Teeth naturally shift over time due to physiological remodeling and aging processes. Retention strategies aim to maintain achieved alignment and reduce relapse tendencies.
Long term stability of Malocclusion correction depends on growth completion, periodontal health, and consistent follow up. Studies suggest that minor positional changes can occur even years after orthodontic therapy. This dynamic aspect highlights the biological adaptability of dental structures.
Ongoing research explores predictive modeling and genetic indicators that may improve future stability outcomes for Malocclusion. As orthodontic science advances, greater precision in individualized planning may enhance long term predictability.
A Comprehensive Perspective on Malocclusion
Malocclusion represents a convergence of developmental biology, functional biomechanics, and aesthetic perception. It is not merely a matter of crooked teeth but a reflection of how jaws grow, how teeth erupt, and how structural balance is maintained over time. The types of Malocclusion illustrate the diversity of bite relationships, while its causes reveal the interplay between heredity and environment.
From diagnostic evaluation to financial considerations, Malocclusion encompasses scientific complexity and practical decision making. Continued research in craniofacial development and orthodontic innovation expands understanding of this condition. By examining its types, causes, expenses, and broader implications, individuals gain a deeper awareness of Malocclusion within the context of oral health science.